- *Corresponding Author:
- X. Song
Department of Spine Surgery, The First Affiliated Hospital, University of South China, Hengyang, Hunan, People's Republic of China
E-mail: belinde666@21cn.com
| This article was originally published in a special issue, "Clinical and Experimental Studies on Drug and Intervention Repurposing in China |
| Indian J Pharm Sci 2019:81(4)spl issue1;129-133 |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
Traditional L5-S1 axial fixation is lack of antirotation biomechanical stability. As a new axial fixation for lumbosacral spine, the antirotation biomechanical stability of L5-S1 locking axial fixation with inner poke has not been verified. Six normal human fresh cadaver lumbosacral spine specimens (L3-S5) were used to construct spondylolysis model by osteotome successively, and then, the six specimens were subjected to L5-S1 axial fixation (control group), L5-S1 locked axial fixation with inner poke (experimental group 1), L5-S1 locked axial fixation with inner poke combine with pedicle screw fixation (experimental group 2) and L5-S1 axial fixation combine with pedicle screw fixation (experimental group 3), respectively, and the range of motion of L5-S1 segment were measured under axial rotation state with maximum torque is 10 Nm. All rotation tests were performed by the spine 3-dimensional motion machine. The results showed that the specimens of control group resulted in more range of motion than other experimental groups in axial rotation. Compared to the traditional axial fixation , the total rotation range of motion of L5-S1 locked axial fixation with inner poke group was significantly decreased (t=-5.065, P=0.04). When L5-S1 locked axial fixation with inner poke combined with pedicle screw fixation, the total rotation range of motion was smaller significantly (t=4.39, P=0.007). The rotation range of motion of experimental group 2 is the smallest in all groups. In conclusion, L5-S1 locking axial fixation with inner poke allowed less rotational motion compared to the traditional axial fixation on the fixed segment and supplied with pedicle screws can improve its performance further in the term of antirotation. The results of this study showed that L5-S1 locking axial fixation with inner poke can improve antirotation function of the traditional axial fixing screw.
Keywords
Lumbosacral vertebrae, axial fixation, locking, antirotation, biomechanics
Lower back pain is mainly caused by lumbosacral degenerative diseases and has threatened people’s health for a long time[1]. The gold standard for treating lumbosacral degenerative diseases is lumbosacral interbody fusion[2]. The surgical methods for fusion are diverse, however, most operations are open and have many shortages such as surgical trauma, destruction of spinal posterior structure, complication and so on. Percutaneous axial lumbosacral interbody fusion (AxiaLIF) was raised by Cragg et al. in 2004[3]. An axial screw was used to fix L5-S1 vertebra percutaneously through the pre-sacral space in the AxiaLIF, which can not only reduced the surgical trauma but also preserved the integrity of spinal structure. Meanwhile, the axial screw improves the stiffness of spine and provides a more stable biomechanical environment for lumbosacral portion[4]. With progress of the biomechanical research on AxiaLIF, the shortcomings of this operation are gradually exposed. It has reported that although AxiaLIF enhanced the stiffness of the spine and the stability in the direction of flexion, extension and lateral bending is superior to the traditional pedicle screw fixation, the antirotation stability is inferior to the traditional fixation[5]. Another study suggested that AxiaLIF combined with posterior pedicle screw fixation could enhance the stability of the fixed segment further and increase the fusion rate[6]. Therefore, AxiaLIF is often used in combination with posterior pedicle screws to ensure adequate stability in clinical[7,8]. However, this combined operation is cumbersome, and employ more internal fixations, which enlarges the surgical trauma and increases the hospitalization cost, so the application of AxiaLIF is heavily restricted in clinical practice at present. In order to improve the antirotation performance of AxiaLIF to expand the scope of clinical application, two inner poke structures based on the traditional axial screw were designed to facilitate locking after axial fixation. The biomechanical test was carried out for evaluating the antirotation stability of L5-S1 locking axial fixation with inner poke, and guiding its further improvement and clinical application.
The study was approved by Ethics Committee of University of South China. All 6 specimens are provided by anatomy laboratory of the University of South China (3 male, 3 female), and the age ranged from 23-65 y. Before the test, all specimens were quantified using X-ray and bone mineral density analysis to exclude congenital malformations, tumours, fractures, severe osteoporosis and other diseases. The lumbosacral motion segments (L3-S5) were cut out, and each specimen was stored at –20°.
It would take about 12 h to unfreeze the specimen before experiment. Soft tissues such as paravertebral muscles were removed, and all ligaments, intervertebral discs, facet joint capsules and bony structures were preserved, and the anterior longitudinal ligament, posterior longitudinal ligament, supraspinous ligament, and interspinous ligament were intact[9]. Both ends of the specimen (L4 and S1 level) should be trimmed, and then the specimen was embedded at both ends by denture base polymer powder to facilitate biomechanical testing. The physiological curvature of the spine was maintained during the embedding process. The force surfaces need to keep basically parallel (fig. 1).
The fixations used in the experiment included L5-S1 locking axial fixation with inner poke (fig. 2), posterior screw-rod system and axial screw (Watson Medical Company, Changzhou, China). The test equipment was spinal 3-dimension motion machine, and be equipped with opting track motion measure system (Optotrak Certus, Northern Digital, Waterloo, Canada), digital X-ray machine, and conventional surgical instruments. A, B L5-S1 locking axial fixation with inner poke, a. the axial screw with a passage for inserting pokes, b. poke for L5, C. poke for S1, d. locking screw, C. installation tools.
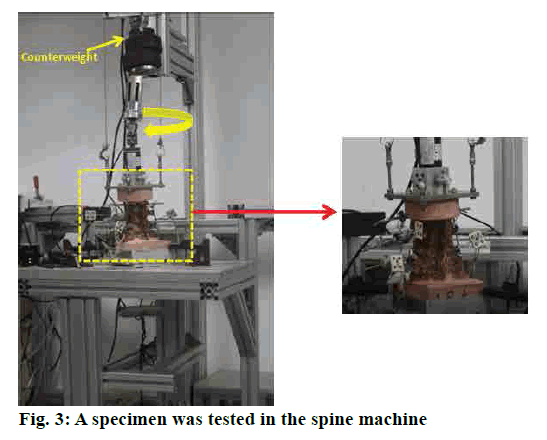
Biomechanical testing was conducted on the customdesigned spine testing machine (fig. 3)[10]. The S1-5 was embedded and secured to the table of the testing machine. The L3 was connected to the loading arm that applied a pure moment to the specimen, and the specimen was allowed to move in an unconstrained rotational fashion[11]. A pure moment of 10 Nm was applied in left and right axial rotation[5].
The specimen is shown in the rotation configuration. The pure moment 10 Nm was applied to the specimen through a loading arm which consisted of a servomotor, gear, two U-joints, a linear bearing and a torque load cell. Six specimens were cleaved the L5-S1 bilateral isthmus to make the posterior column instability model by using the osteotome. And then, each of the L5/S1 spondylolysis specimens undergone the four different conditions, randomly L5-S1 axial fixation (control group, CG), L5-S1 locking axial fixation with inner poke (experimental group 1, EG1), L5-S1 locking axial fixation with inner poke and pedicle screw fixation (experimental group 2, EG2), L5-S1 axial fixation and pedicle screw fixation (experimental group 3, EG3).
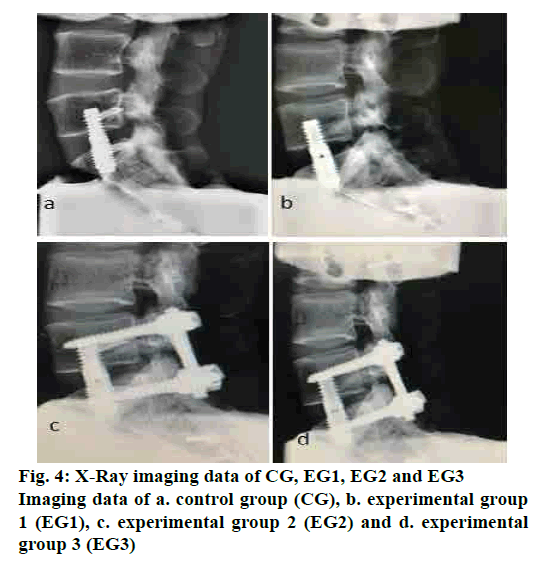
For installing the axial screw, take the upper point of the S1/2 transverse line as the entry point, the axial screw was placed into the L5 and S1 vertebral body and the direction is perpendicular to the end plate of the L5[12]. The two pokes were inserted into the L5 and S1 body through the passage of the screw in EG1, without penetrating the cortical bone. The posterior pedicle screw fixation was implanted in EG2 and EG3 respectively. After installation of fixations, all specimens examined by X-Ray (fig. 4).
The L5/S1 spondylolysis with axial screw a. CG; b. EG1, the specimens are L5/S1 spondylolysis with L5-S1 locking axial fixation with inner poke; c. EG2, the specimens are L5/S1 spondylolysis with L5-S1 locking axial fixation with inner poke and pedicle screw fixation; d. EG3, the specimens are L5/S1 spondylolysis with L5-S1 axial screw and pedicle screw fixation (n=6).
There are 3 markers on L4, L5 and S1 vertebrae respectively. The Optotrack system will measure the range of motion (RoM) of the L5/S1 segment through recording the movement of markers, when the specimen is under the state of axial rotation (figs. 4 and 5). During the experiment, the surface of the specimen was sprayed with normal saline to keep it moist[13]. The room temperature was kept at 20-25°.
The statistical data of the experimental data were analysed by SPSS19.0 software. Paired t-test was used to compare the different groups. P<0.05 indicates that the difference was statistically significant significance.
The rotation RoM of the 4 groups was showed in Table 1, the unit of RoM is degree (°). Compared with CG, the rotation RoM of EG1 is smaller and the difference is statistically significant. Compared with EG2 and EG3, respectively, the rotation RoM of CG is larger and the difference is statistically significant. Compared with EG2 and EG3, respectively, the rotation RoM of EG1 is larger and the difference is statistically significant. On comparison between EG2 and EG3, the rotation RoM of EG2 is smaller, and there is no statistically significance. The left and right rotation RoM of EG1 was no statistically significance (p>0.05).
| CG | EG1 | EG2 | EG3 | |
|---|---|---|---|---|
| Right rotation | 3.33 (1.16) | 2.65 (1.12) | 0.85 (0.45)ab | 0.93 (0.62)ab |
| Left rotation | 3.37 (2.02) | 2.66 (1.11) | 0.94 (0.41)ab | 1.17 (0.51)ab |
| Total rotation | 6.70 (2.78) | 5.31 (2.22)a | 1.79 (0.85)ab | 2.10 (1.12)ab |
Data are mean (SD). aSignificant difference from CG; bsignificant difference from EG1 (p<0.05)
Table 1: Rotation ROM of four groups
The FSU (function of spinal unit) is composed of upper and lower vertebral bodies, intervertebral discs and intervertebral facets, also known as the motion segment of the spine. It is because of this special structure that the spine can complete the movement of the six directions of flexion and extension, right and left side bending, and left and right rotation. On the contrary, the threejoint complex which is made up of the intervertebral facet joints on both sides of the motion segment, and the intervertebral disc can prevent the spine from excessive movement[14]. The intervertebral facet joints play an important role in spinal antirotation function[15]. Under physiological condition, these structures maintain the normal motion of the spine. However, with the increase of age and the stress changes of spine, the intervertebral disc and intervertebral facet joints are degenerating gradually, and the stable state of spinal motion has been broken. Especially in the spinal stress concentration area-lumbosacral segment, the spinal instability is more likely to occur, and the instability will cause the symptom such as low back pain at last.
AxiaLIF is mainly used in the treatment of lumbosacral degenerative diseases, such as lumbar instability, mild lumbar spondylolisthesis[16]. The pain symptoms of these diseases are primarily result from the instability of the lumbosacral vertebrae. The main treatment for this kind of diseases is intervertebral fusion, and stable biomechanical environment is one of the basic conditions for fusion[17]. Among all kinds of lumbosacral fusion operations, the advantages of AxiaLIF are less trauma for muscle and ligament and preservation for the posterior components of the spine[18]. However, the past biomechanical studies on L5/S1 axial fixation have showed that even though the axial fixing screws can provide sufficient resistance to flexion and extension and lateral bending motion, the antirotation stability is still insufficient[5]. Another study reported that AxiaLIF supplemented with posterior pedicle screw fixation can enhance the biomechanical stability for the fixed segment, which also ensures the fusion success rate[19]. But the combination with the posterior pedicle screw fixation also covered the unique advantages of minimally invasive surgery in AxiaLIF. In the present study, we have examined the biomechanical function of L5-S1 Locking Axial Fixation with Inner Poke in term of antirotation, which could maintain the minimal invasive advantages of AxiaLIF, and improve the antirotation stability of the traditional axial screw also, the present study maybe expand the clinical application range of AxiaLIF.
It is well known that the traditional axial screw just fixes the anterior and middle columns of the spine. Therefore, when motion segment lost the restriction of intervertebral joint, or the posterior column of the spine became unstable, AxiaLIF cannot provide enough antirotation stability for the segment. And insufficient strength for fixation will inevitably affect the success rate of intervertebral fusion. The L5-S1 locking axial fixation with inner poke improved on the basis of the traditional axial fixing screw by adding two thornlike structures which can be inserted from the original channel. The two pokes are protruded from the axial screw and are unidirectionally locked in the L5 and S1 vertebral bodies. The vertebral cortical bone is not penetrated, and the two internal thorn structures are perpendicular to the central axis of the spine, which are fixed in the axial screw after locking (fig. 4b). The rotational motion of the lumbosacral segment will significantly increased when the posterior column of the spine becomes unstable. So the spondylolysis model was constructed to accept 4 sorts of fixation and via biomechanical examination to observe the limitation on rotational motion of each fixation. The rotation RoM of the EG1 was significantly smaller than CG, which indicated the L5-S1 locking axial fixation with inner poke could significantly improve the antirotation stability of the traditional axial fixation. Compared with the EG2 and the EG3, the rotation RoM of EG1 was significantly bigger than these two groups, which suggested that the axial fixation combined with the posterior pedicle screw fixation provided more antirotation stability for the spine. The rotation RoM of EG2 was smaller than EG3, however, there was no statistically significance difference, it may be due to the fact that the posterior pedicle fixation had a stronger restriction on the rotational motion of the spine, which might cover up the antirotation effect of the locking axial screw with inner poke.
In conclusion, the L5-S1 locking axial fixation with inner poke can limit the rotation motion better than traditional axial fixation on spondylolysis model, meanwhile, it has preserved the advantages of traditional AxiaLIF, such as smaller trauma, quicker recovery, the stronger stiffness of the spine, and preservation of the integrity of the spinal posterior column. This study has proved that the L5-S1 locking axial fixation with inner poke has a better antirotation function than traditional axial fixation and could provide comprehensive experimental data and reliable theoretical basis for the clinical application of single axial lumbosacral fixation without posterior fixation.
Acknowledgements:
This work was supported by the National Science Foundation of China (81272055).
Conflicts of interest:
None of the authors has financial or other conflicts of interest concerning this study.
References
- Zhang X, Hao J, Hu Z, Yang H. Clinical Evaluation and Magnetic Resonance Imaging Assessment of Intradiscal Methylene Blue Injection for the Treatment of Discogenic Low Back Pain. Pain Physician 2016;19:1189-95.
- Schroeder, GD, Kepler CK, Millhouse PW, Fleischman AN, Maltenfort MG, Bateman DK, et al. L5/S1 Fusion Rates in Degenerative Spine Surgery A Systematic Review Comparing ALIF, TLIF, and Axial Interbody Arthrodesis. Clin Spine Surg, 2016;24:201-18.
- Cragg A, Carl A, Casteneda F, Dickman C, Guterman L, Oliveira C. New percutaneous access method for minimally invasive anterior lumbosacral surgery. Spinal Disord Tech 2004;17:21-8.
- Marotta N, Cosar M, Pimenta L, Khoo LT. A novel minimally invasive presacral approach and instrumentation technique for anterior L5-S1 intervertebral discectomy and fusion. Neuro Surg Focus 2006;20:9-17.
- Ledet, EH, Tymeson MP, Salerno S, Carl AL, Cragg A. Biomechanical evaluation of a novel lumbosacral axial fixation device. J Biomech Eng 2005;127:929-33.
- Akesen B, Wu C, Mehbod AA, Transfeldt EE. Biomechanical evaluation of paracoccygeal transsacral fixation. J Spinal Disord Tech 2008;21:39-44.
- Aryan HE, Newman CB, Gold JJ, Acosta FL, Jr. Coover C, Ames CP. Percutaneous axial lumbar interbody fusion (AxiaLIF) of the L5-S1 segment: initial clinical and radiographic experience. Minim Invasive Neurosurg 2008;4:225-30.
- Bohinski RJ, Jain VV, Tobler WD. Pre-sacral retroperitoneal approach to axial lumbar interbody fusion: a new, minimally invasive technique at L5-S1: Clinical outcomes, complications, and fusion rates in 50 patients at 1-year follow-up. SAS J 2010;4:54-62.
- Zhou RZ, Huang ZP, Liu X, Tong J, Ji W, Liu ST, et al. Kinematics and load-sharing of an anterior thoracolumbar spinal reconstruction construct with PEEK rods: An in vitro biomechanical study. Clin Biomechanics 2016;40:1-7.
- Dvorak MF, Sekeramayi F, Zhu Q, Hoekema J, Fisher C, Boyd M, et al. Anterior occiput to axis screw fixation: part II: a biomechanical comparison with posterior fixation techniques. Spine 2003;28:239-45.
- Zhu Q, Larson CR, Sjovold SG, Rosler DM, Keynan O, Wilson DR, et al. Biomechanical evaluation of the total facet arthroplasty system: 3-dimensional kinematics. Spine 2007;32:55-62.
- Liu BF, Zhang LG, Liu YB, Yan N, Zhang HL, Gu X, et al. Is the trans-sacral axial interbody fusion a candidate surgical approach for fusing both L5 /S1 and L4. Chin Med J 2011;124:215-7.
- Wilke HJ, Wenger K, Claes L. Testing criteria for spinal implants: recommendations for the standardization of in vitro stability testing of spinal implants. Eur Spine J 1998;7:148-54.
- Jaumard NV, Welch WC, Winkelstein BA. Spinal facet joint biomechanics and mechanotransduction in normal, injury and degenerative conditions. J Biomech Eng 2011;133:58 -63.
- Kalichman L, Hunter DJ. Lumbar facet joint osteoarthritis: a review. Semin Arthritis Rheum 2007;37:69-80.
- Mazur MD, Duhon BS, Schmidt MH, Dailey AT. Rectal perforation after AxiaLIF instrumentation: case report and review of the literature. Spine 2013;13:29-34.
- Burkus JK. Surgical treatment of the painful motion segment: matching technology with indications. Spine 2005;30:7-15.
- Hofstetter CP, James AR, Härtl R. Revision strategies for AxiaLIF. Neurosurg Focus 2011;31:17-24.
- Beaubien BP, Derincek A, Lew WD, Wood KB. In vitro, biomechanical comparison of an anterior lumbar interbody fusion with an anteriorly placed, low-profile lumbar plate and posteriorly placed pedicle screws or translaminar screws. Spine 2005;30:1846-51.