- *Corresponding Author:
- Yanyan Xiao
Department of Pediatrics,
The Third Affiliated Hospital,
Hengyang Medical School,
University of South China,
Hengyang,
Hunan 421900,
China
E-mail: feiyanfeiyan2021@163.com
| This article was originally published in a special issue, “Trending Topics in Biomedical Research and Pharmaceutical Sciences” |
Indian J Pharm Sci 2022:84(1) Spl Issue “196-203” |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
To investigate the efficacy of color Doppler ultrasound combined with propranolol in the treatment of infantile vascular cancer is the objective of the study. 126 children with vascular cancer in the Department of Dermatology of a provincial hospital were randomly divided into ultrasound, propranolol and conventional systematic treatment. Compared with the control group, the experimental group could master more detailed and comprehensive information on the volume, depth and elasticity of hemangioma and the size of hemangioma in the experimental group decreased by 38.5 % after 1 mo of treatment and 59.7 % after 3 mo of treatment. The coagulation function of blood vessels recovered and the blood flow velocity increased by 22.3 % compared with that before treatment. The effect of rehabilitation treatment was significantly better than that of the control group (76.49 %>62.35 %). There was significant difference between the two groups in adverse reactions such as blister (p=0.146), infection (p=0.027), pigment change (p=0.033), scar (p=0.032) and rash (p=0.007) (p<0.05). The average treatment effect of vascular cancer in the experimental group was 94.55 %, which had significant statistical significance in the recovery of physical function and coordination of patients (p<0.05), and the median survival time and quality of life were significantly different from those in the control group (p<0.05). Ultrasound combined with propranolol can effectively improve the condition of infant vascular cancer, contribute to the later rehabilitation treatment and improve the quality of life.
Keywords
Color Doppler ultrasound, propranolol, cutaneous hemangioma, image features, blood flow velocity
Cutaneous hemangioma is a congenital disease showing tumor and vascular malformation due to the abnormal development of vascular endothelial tissue and surrounding tissues during embryonic development. It is usually divided into fresh erythema nevus, cavernous hemangioma, mixed hemangioma, etc. The probability of infants suffering from cutaneous hemangioma accounts for 4 %-5 % of their births [1-3]. Patients with cutaneous hemangiomas of different shapes and different course of disease also suffer from different problems. 50 % of hemangiomas will subside by themselves, but the degree of regression is limited. Affected by individual physical differences, the residual fibrous tissue will affect the aesthetic feeling and affect the mental and psychological health of patients and their families [4]. Some hemangiomas will have complications such as rupture, bleeding and scar during the course of the disease, while common treatment methods such as freezing, radiation therapy and hormone oral drug treatment have poor curative effect and obvious side effects, poor drug safety performance and will cause skin necrosis and allergy to the growth and development of infant patients [5,6].
Color Doppler ultrasound treatment is an ideal treatment method. The ultrasound treatment can scan the tumor from multiple angles, has the advantages of noninvasive and safe, can accurately detect the lesion range, evaluate the pathological changes of the tumor, and reduce the surgical risk caused by conventional laser treatment. Propranolol can effectively reduce the effect of vascular endothelial growth factor, inhibit the expansion of hemangioma, improve the patient’s condition and promote the rehabilitation of the diseased site [7,8]. Therefore, this paper explores the efficacy of color Doppler ultrasound combined with propranolol in the treatment of infantile hemangioma, so as to provide positive and effective treatment schemes and suggestions for the treatment of infantile hemangioma.
Materials and Methods
General information:
126 children with vascular cancer in the dermatology department of a provincial hospital were selected. The diagnosis of the disease was confirmed by the deputy chief physician and met the standards of skin pathology. Ethics committee approval was obtained from the Institutional Ethics Committee of The Third Affiliated Hospital, Hengyang Medical School, University of South China to the commencement of the study. Before treatment, all children underwent three routine examinations of hematuria and stool and functional examinations such as contraindication of drug-resistant components, so as to avoid abnormal interference factors in the experimental operation. Before treatment, they indicated the possible adverse reactions, prognostic consequences and treatment risks during the medication period to the patient’s family members, and signed the informed consent after obtaining their consent. The patients were randomly divided into experimental group and control group. In the control group, routine treatment methods were used for intervention according to the clinical experience of therapists and the data related to condition of patients in the process of treatment were recorded by conventional instruments. The experimental group was treated with color Doppler ultrasound and propranolol. Before the experiment, the age, course of disease, degree and type of hemangioma, blood flow velocity and other basic information and condition of the patients were statistically sorted. The results are shown in Table 1.
| Hemangioma | Number of cases | Age (mo) | Lesion area | Rash depth | Blood flow velocity | |
|---|---|---|---|---|---|---|
| Type | Superficial phenotype | 80 (68.96 %) | 6.83±6.79 | 8.95±5.74 | 3.53±1.18 | 16.41±11.75 |
| Deep type | 26 (22.41 %) | 4.49±3.52 | 5.34±4.12 | 4.62±2.01 | 15.39±10.67 | |
| Mixed type | 10 (8.63 %) | 5.26±4.68 | 6.77±4.80 | 4.22±1.76 | 16.23±11.39 | |
| Site | Head and face | 53 (45.68 %) | 5.77±5.26 | 4.58±1.49 | 3.47±1.15 | 17.23±12.16 |
| Trunk | 33 (28.44 %) | 5.46±3.45 | 7.43±3.26 | 3.39±1.13 | 15.33±10.98 | |
| Limb | 30 (25.88 %) | 7.26±1.28 | 7.96±2.15 | 3.51±1.22 | 16.28±11.57 | |
Table 1: Basic Information of The Patient
In Table 1, the hemangioma types of patients are mainly shallow phenotypes, which are mostly found in the head, face and trunk. There is no difference in age, disease location and type, blood flow velocity and other indicators, which is not statistically significant, so the later experiment can be carried out.
Research methods and index selection:
There are many causes and types of skin vascular cancer. Vascular cancer with different shapes and areas has great differences in the distribution of subcutaneous tissue and the detection of blood flow velocity. The lesion volume, depth, blood flow velocity, thrombin and elasticity index of hemangioma were detected by Doppler ultrasound and Computed Tomography (CT), to master the changes of hemangioma [9,10]. At the same time, the treatment efficacy was evaluated on the adverse reactions of patients, the satisfaction of patient’s family members and the survival of patients after treatment, that is, the grade was divided by recording the size, surface tension and color changes of hemangioma. The tumor shrinkage or surface color regression of 76%-100% was significantly effective and the tumor shrinkage or surface color regression of 35 %-75 % was partially effective. It is invalid if the tumor shrinks or the surface color fades by 0%-34% [11,12].
Statistical methods:
Statistical Package for the Social Sciences (SPSS) 22.0 was used where statistical software arranges and analyzes the experimental data. If the measurement data conforms to the normal distribution, it is expressed in the form of mean±standard deviation, i.e.x̄±s; the comparison between groups was carried out by t-test. If the data did not conform to the normal distribution, it was expressed by quartile and median, and U-test was used. The counting data are expressed by column number or percentage, and χ2 or Mann Whitney U test formula is used, p<0.05 indicates that the data have obvious statistical difference [13].
Results and Discussion
Analysis of observation results of hemangioma by different testing machines was shown below. The experimental group used Doppler ultrasound to detect hemangiomas and the control group used conventional CT to detect hemangiomas. The detection results of some hemangiomas are shown in fig. 1.
Fig. 1 shows the detection results of superficial and mixed skin vascular cancer. It can be seen that ultrasound can better grasp the volume and range of vascular cancer. At the same time, the volume of hemangioma, Peak Systolic Velocity (PSV) of blood flow, Resistance Index (RI) of blood flow and elasticity index of hemangioma under different treatment schemes are statistically analyzed. The results are shown in Table 2.
It can be seen from Table 2 that the experimental group detected by Doppler ultrasound has better detection effect on the lesion volume, depth, blood flow velocity and elasticity index of hemangioma than the control group detected by CT and the ultrasonic detection has significant statistical significance on the volume, depth and elasticity of deep hemangioma and mixed hemangioma (p<0.05), grasp the patient’s condition in more detail.
| Index | Superficial phenotype | Depth type | Mixed type | |||
|---|---|---|---|---|---|---|
| Experimental group | Control group | Experimental group | Control group | Experimental group | Control group | |
| Lesion volume (cm2) | 9.23±5.74 | 8.95±5.69 | 6.99±4.12* | 5.34±4.17 | 8.13±4.06* | 6.77±4.80 |
| Hemangioma depth (mm) | 3.25±1.12 | 3.17±1.08 | 4.28±2.01* | 2.13±1.14 | 3.79±1.45* | 1.58±1.21 |
| Blood flow velocity (cm/s) |
15.38±11.79 | 16.41±11.75 | 15.78±14.98 | 15.39±10.67 | 17.34±13.03 | 16.23±11.39 |
| Elasticity index | 1.24±1.17 | 1.15±1.09 | 2.74±1.19* | 1.23±1.09 | 1.96±1.05* | 1.47±1.01 |
Note: *means p<0.05 compared with the control group
Table 2: Comparison of Hemangioma Detection Results Between The Two Groups
Analysis of therapeutic effects of different treatment methods on patients with hemangioma was described below. The experimental group was treated with propranolol and the control group was treated with conventional sebum drugs. At the same time, the curative effects of the two groups before and after treatment were counted with the help of detection image tools. The results are shown in Table 3.
| Index | Before treatment | 1 mo after treatment in the experimental group | 3 mo after treatment in the experimental group | 1 mo after treatment in the control group | The control group was treated for 3 mo |
|---|---|---|---|---|---|
| Volume | 6.89±3.77 | 4.19±2.65* | 2.76±1.94*# | 6.17±2.65* | 5.26±1.03 |
| PSV | 69.86±15.13 | 53.54±12.11* | 39.17±9.85*# | 65.42±16.01* | 58.74±11.63 |
| RI | 0.62±0.15 | 0.85±0.14* | 0.99±0.11*# | 0.68±0.05* | 0.79±0.12 |
| Elasticity index | 2.68±1.24 | 2.98±1.11* | 3.01±0.85* | 2.71±1.22 | 2.96±0.69 |
Note: *means p<0.05 compared with that before treatment; *#means p<0.05 compared with the control group
Table 3: Analysis of The Effect of Ultrasound Image Before and After Treatment of Hemangioma With Different Drugs
In Table 3, the changes of hemangioma volume, PSV, RI and elastic index of the two groups after drug treatment are statistically significant compared with those before treatment (p<0.05), but with the increase of treatment cycle, the curative effect of the experimental group is statistically significant compared with that of the control group (p<0.05). It has a good effect on restoring the elasticity of skin tissue. At the same time, the rehabilitation and adverse reactions of patients after treatment are sorted out. The results are shown in fig. 2. It can be seen from fig. 2 that the rehabilitation and adverse reactions of patients with vascular cancer after different treatment methods are different. Fig. 2a shows the cure of the two groups after treatment. The rehabilitation of the patients in the experimental group is significantly better than that in the control group (76.49 %>62.35 %) and the data of the two groups have significant statistical difference (p<0.05). In fig. 2b, the two groups of patients had different proportions of adverse reactions such as blisters (25.2 % in the experimental group and 27.3 % in the control group, p=0.146), infection (4.2 % in the experimental group and 7.9 % in the control group, p=0.027), pigment changes (54.3 % in the experimental group and 69.8 % in the control group, p=0.033), scars (16.5 % in the experimental group and 32.1 % in the control group, p=0.032) and rash (58.3 % in the experimental group and 72.4 % in the control group, p=0.007). The recurrence rate of adverse reactions in the experimental group was significantly lower than that in the control group and the difference between color sink of scar and rash was the largest. The treatment data of the two groups had significant statistical significance (p<0.05), indicating that different treatment methods had different therapeutic effects on vascular cancer. At the same time, explore the relationship between the treatment effect of the experimental group and the type and growth site of vascular cancer, and sort out the statistics. The results are shown in Table 4.
| Classification | Number of cases | Curative effect | Chi square test | ||||
|---|---|---|---|---|---|---|---|
| Significantly effective | Partially valid | Invalid | X2 | p | |||
| Type | Superficial phenotype | 80 | 45 | 33 | 2 | 4.835 | 0.308 |
| Deep type | 26 | 4 | 21 | 1 | |||
| Mixed type | 10 | 2 | 7 | 1 | |||
| Position | Head, face and neck | 53 | 14 | 38 | 1 | 3.768 | 0.584 |
| Body cadre | 33 | 23 | 9 | 1 | |||
| Limb | 30 | 17 | 13 | 0 | |||
Table 4: The Relationship Between The Therapeutic Effect and The Type and Growth Site of Vascular Cancer in The Experimental Group
In Table 4, it is found that there is significant statistical significance between the treatment effect and the type of vascular cancer in the experimental group (χ2= 4.835, p=0.308), and the effective rates for superficial vascular cancer, deep vascular cancer and mixed vascular cancer are 97.5 %, 96.15 % and 90 % respectively. However, there is no significant statistical significance between the treatment effect and the location of vascular cancer in the experimental group (p=0.584>0.05), but the diseased sites are trunk, the effective rates of limbs were still 26.42 % and 69.69 %. The reason is that ultrasound can more carefully and comprehensively check the affected area, so that doctors can better grasp the relevant information of patients with vascular cancer, timely record the changes of patient’s lesion sites and the suitability of drugs and avoid the damage of normal tissues caused by excessive treatment while obtaining curative effect [14-16]. After adjusting the dosage, the patient’s condition changes are recorded and the results are shown in Table 5.
| Index | Volume | Plasma thrombin time | RI | Elasticity index |
|---|---|---|---|---|
| Before treatment | 6.97±3.89 | 16.5±0.25 | 0.60±0.13 | 2.72±1.21 |
| 1 mo later | 4.28±2.79* | 12.4±1.03* | 0.74±0.12* | 2.82±1.07 |
| 3 mo later | 2.83±1.97# | 11.7±0.53# | 0.85±0.12# | 2.93±0.81 |
| T1 | 3.07 | 4.21 | 4.14 | 0.34 |
| F1 | 3.21 | 1.49 | 1.04 | 0.98 |
| T3 | 2.31 | 5.08 | 3.68 | 4.40 |
| F3 | 1.31 | 0.04 | 0.14 | 2.07 |
Note: *means p<0.05 compared with that before treatment; #means p<0.05 compared with that 1 mo after treatment
It can be seen from Table 5 that the changes of patient’s condition after treatment with propranolol have changed in various indexes. The improvement of hemangioma volume, thrombin time, RI and elasticity index in the 1st mo and 3rd mo after treatment is statistically significant compared with that before treatment (p<0.05), in which the hemangioma volume has decreased by 38.5 % after 1 mo of treatment, After 3 mo of treatment, it is decreased by 59.7 % compared with the 1st mo. The coagulation function of blood vessels has recovered and the thrombin time has recovered from 11 s-13 s after treatment. RI increased by 22.3 % after 1 mo of treatment and 41.7 % after 3 mo of treatment. It shows that the drug treatment can better improve the blood flow, relieve the obstruction of blood flow and then reduce the risk of aggravation.
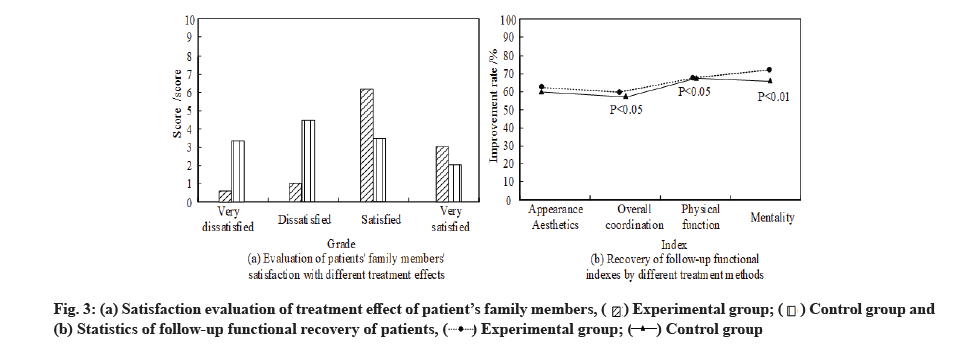
Analysis of patient’s satisfaction and treatment effect after treatment was described below. The rehabilitation and satisfaction scores of patients with different treatment schemes are counted and the results are shown in fig. 3.
Fig. 3 shows the satisfaction score of the patient’s family members on the treatment effect and the functional recovery of the patient after treatment. In fig. 3a, the family members of the patients in the experimental group have a high score on the treatment effect and the average score of satisfaction is 5.73 points, and the score of dissatisfaction is only 0.54 points, while the average score of satisfaction in the control group is less than that of dissatisfaction (3.36 points<4.28 points). In fig. 3b, the improvement rate of wound appearance, physical function and psychological state of the experimental group is higher than that of the control group, and the recovery and coordination of the overall function of the patients in the experimental group are greatly improved, and the difference is statistically significant (p<0.05). At the same time, the better treatment effect of the experimental group on patients condition can better make up for patients defects and has a better positive effect on their subsequent physical and mental growth and maintenance of mental health. Compared with the control group, the value has a very significant statistical significance (p<0.01). Regular follow-up visits and condition records are made for patients, and the follow- up treatment process and rehabilitation of patients are sorted out. The results are shown in Table 6.
| Therapeutic time | Time group | Grouping | Censored data (%) |
Median survival time (mo) | 95 % confidence interval (mo) |
|---|---|---|---|---|---|
| ≤3 mo | 1-30 d | Control group | 1 (1.4) | 2.5 | 2-3 |
| Experimental group | 3 (2.3) | 3.5 | 3-4 | ||
| Log rank (Mantel-Cos), X2=55.13, p=0.042 | |||||
| 31-90 d | Control group | 2 (2.6) | 3 | 2.5-4.5 | |
| Experimental group | 8 (13.3) | 8 | 7.5-9.5 | ||
| Log rank (Mantel-Cos), X2=69.082, p=0.000* | |||||
| >3 mo | 90-120 d | Control group | 1 (4.2) | 4 | 1-7 |
| Experimental group | 4 (8.5) | 20 | 17-23 | ||
| Log rank (Mantel-Cos), X2=7.289, p=0.031* | |||||
| ≥121 d | Control group | 2 (10.8) | 5 | 3-7 | |
| Experimental group | 6 (23.1) | 56 | 45-112 | ||
| Log rank (Mantel-Cos), X2=4.186, p=0.001* | |||||
Table 6: Analysis of Survival Results of Patients Under Different Treatment Methods
It can be seen from Table 6 that when the time is within 1 mo, there is no significant difference in the survival time between patients taking propranolol and patients taking conventional hormone drugs. The median survival time of the experimental group and the control group are 2.5 mo and 3.5 mo respectively, and the cumulative survival time between them is statistically significant (χ2=55.13, p=0.042<0.01). When the time was 2 mo, the difference of median survival time between the two groups was further widened and the statistical significance was more significant (p=0.000<0.01), when the later medication time exceeds 3 mo, the median survival time of patients in the control group increases slightly, with the maximum increase of 1.5 mo. The reason may be that the patients have drug resistance, so the follow- up treatment effect is not obvious and the survival time is short [17]. The cumulative survival time of patients in the experimental group was increasing and there was significant statistical significance compared with that in the control group (p<0.01).
Environmental pollution and unsafe food hygiene will increase various risks of pregnant women during pregnancy, causing the rising prevalence of neonatal hemangioma. Skin vascular cancer in exposed and important parts will also affect the patient’s local physical function and appearance. For example, some diseased vascular cancer parts are near the lips, nose, eyes and lateral ears, the spread of the disease will affect the normal operation of organs and the development of nervous system. At the same time, some problems such as large-area scars and fibrous tissue hyperplasia after surgical treatment will also affect the psychological status of infants [18-20]. There are some problems such as poor effect of common surgical schemes on the detection and treatment of hemangiomas. The inner walls of some thicker hemangiomas are of different sizes and irregular shapes. It is difficult to detect the condition better and completely by traditional CT detection, so it is difficult to grasp the changes of symptoms. There are no recognized characteristics to evaluate the degradation rate and degradation process of hemangiomas, the best treatment for hemangioma depends on its course [21].
With the introduction of the new instrument, ultra wideband images are extended to vascular surgery. Doppler ultrasound can better display the condition of vascular cancer with complex internal structure, small volume and small area. Propranolol is a selective drug commonly used in clinical treatment of heart diseases such as hypertension and angina pectoris beta (β) receptor blockers can effectively improve blood flow obstruction [22-24]. Therefore, with the help of Doppler ultrasound and propranolol drug treatment, we can effectively select the appropriate treatment scheme according to individual differences, timely and effectively grasp the changes of vascular cancer condition, and determine the intervention mode and intervention time for a variety of hemangiomas, which can effectively increase the understanding of the natural course of disease and risk prediction, which has important clinical significance.
The results showed that the volume, depth and elasticity of deep hemangioma and mixed hemangioma in the experimental group detected by Doppler ultrasound were more detailed and comprehensive than those in the control group detected by CT (p<0.05). After the intervention with propranolol, it was found that the values of hemangioma volume change, peak blood flow velocity and blood flow RI in the two groups were significantly higher than those before treatment (p<0.05), and the difference in the values of the experimental group was more obvious. The therapeutic effect of propranolol was further explored. It was found that the volume, thrombin time, RI and elasticity index of hemangioma in patients were significantly improved in the 1st mo and 3rd mo after treatment compared with those before treatment. Among them, the size of hemangioma decreased by 38.5 % after 1 mo of treatment and 59.7 % after 3 mo of treatment compared with the 1st mo; the coagulation function of blood vessels has recovered. After treatment, the thrombin time has recovered from the normal range of 11 s-13 s and the result of RI after 1 mo of treatment is 22.3 % higher than that before treatment, and the value after 3 mo of treatment is 41.7 % higher than that after 1 mo of treatment (p<0.05). It shows that the drug treatment can better improve the blood flow velocity and improve the obstruction, so as to alleviate the disease and reduce the disease.
The adverse reactions of patients after treatment were counted and the results showed that the rehabilitation of patients in the experimental group was significantly better than that in the control group (76.49 %>62.35 %), and there were significant differences in blisters (p=0.146), infection (p=0.027), pigment changes (p=0.033), scars (p=0.032) and rashes (p=0.007) between the two groups (p<0.05). With the help of Doppler ultrasound and propranolol drug treatment, the effective rates of superficial vascular cancer, deep vascular cancer and mixed vascular cancer can reach 97.5 %, 96.15 % and 90 %, and the significant effective rates of trunk and limbs can reach 26.42 % and 69.69 %. At the same time, the patients were followed up after treatment, and the results showed that, the family members of the patients in the experimental group had a high score on the treatment effect, the average score of satisfaction was 5.73, and the recovery and coordination of the overall function of the patients were greatly improved. The difference was statistically significant compared with the control group (p<0.05). The rehabilitation and treatment process of the patients showed that when the time was 2 mo, the difference of median survival time between the two groups was further widened and the statistical significance was more significant (p=0.000<0.01). With the increase of time, the median survival time of patients in the control group increased slightly, with the maximum increase of 1.5 mo. The cumulative survival time of patients in the experimental group increased and there was significant statistical significance with the survival time of patients in the control group (p<0.01).
In conclusion, color Doppler ultrasound combined with propranolol can effectively monitor the condition of infant vascular cancer and on this basis, give targeted drug treatment to help them formulate personalized plans. At the same time, drug treatment can effectively control the expansion of lesion area, promote the rehabilitation process, reduce disease recurrence and adverse reactions, greatly improve the quality of life of patients, and provide reference for clinical research.
Conflict of interests:
The authors declared no conflict of interest.
References
- Orbach D, Sparber-Sauer M, Laetsch TW, Minard-Colin V, Bielack SS, Casanova M, et al. Spotlight on the treatment of infantile fibrosarcoma in the era of neurotrophic tropomyosin receptor kinase inhibitors: International consensus and remaining controversies. Eur J Cancer 2020;137:183-92.
[Crossref] [Google Scholar] [PubMed]
- de Kock L, Fahiminiya S, Fiset PO, Astigarraga I, Nguyen VH, Albrecht S, et al. Infantile pulmonary teratoid tumor. N Engl J Med 2018;378(23):2238-40.
[Crossref] [Google Scholar] [PubMed]
- Gomes AP, Germano A, Sousa M, Martins R, Coelho C, Ferreira MJ, et al. Preoperative color Doppler ultrasound parameters for surgical decision-making in upper arm arteriovenous fistula maturation. J Vasc Surg 2021;73(3):1022-30.
[Crossref] [Google Scholar] [PubMed]
- Li M, Li Q, Yin Q, Wang Y, Shang JM, Wang LH. Evaluation of color Doppler ultrasound combined with plasma miR-21 and miR-27a in the diagnosis of breast cancer. Clin Transl Oncol 2021;23(4):709-17.
[Crossref] [Google Scholar] [PubMed]
- O'Bryhim BE, Li AS, Bayliss SJ, Tychsen L, Lueder GT, Rajagopal R. Successful treatment of an exudative choroidal hemangioma with oral propranolol in a 10-year-old boy. J AAPOS 2019;23(4):236-8.
[Crossref] [Google Scholar] [PubMed]
- Risbayevich BS, Aoyama T, Ergashevich MS, Sakamoto J, Shavkatovich BS, Shevket-Oglu YS. Selection of treatment for patients with acute colonic obstruction of tumor etiology. Ann Cancer Res Ther 2019;27(1):15-8.
- Lee HS, Park P, Han S, Joo N, Song YR, Kim JK, et al. Custom-made Doppler ultrasound flow simulator for dialysis access using continuous renal replacement therapy machine. J Vasc Access 2019;20(6):701-5.
[Crossref] [Google Scholar] [PubMed]
- El Kaffas A, Gangeh MJ, Farhat G, Tran WT, Hashim A, Giles A, et al. Tumour vascular shutdown and cell death following ultrasound-microbubble enhanced radiation therapy. Theranostics 2018;8(2):314-27.
[Crossref] [Google Scholar] [PubMed]
- Lövey J, Polgár C. Combination of radiation and immunotherapy in cancer treatment. Magyar onkol 2019;63(3):196-201.
[Google Scholar] [PubMed]
- Roman BR, Randolph GW, Kamani D. Conventional thyroidectomy in the treatment of primary thyroid cancer. Endocrinol Metab Clin North Am 2019;48(1):125-41.
[Crossref] [Google Scholar] [PubMed]
- Morris MA, Ring CM, Managuli R, Saboury B, Mehregan D, Siegel E, et al. Feature analysis of ultrasound elastography image for quantitative assessment of cutaneous carcinoma. Skin Res Technol 2018;24(2):242-7.
[Crossref] [Google Scholar] [PubMed]
- Staackmann C, Schild Se, Rades D. Palliative radiotherapy for cutaneous squamous cell carcinoma of the head-and-neck region. In Vivo 2021;35(4):2283-8.
[Crossref] [Google Scholar] [PubMed]
- García MP, Puchades AM, Jiménez OS. Perineural invasion in cutaneous squamous cell carcinoma. Actas Dermosifiliogr 2019;110(6):426-33.
[Crossref] [Google Scholar] [PubMed]
- Azimi A, Kaufman KL, Kim J, Ali M, Mann GJ, Fernandez-Penas P. Proteomics: An emerging approach for the diagnosis and classification of cutaneous squamous cell carcinoma and its precursors. J Dermatol Sci 2020;99(1):9-16.
[Crossref] [Google Scholar] [PubMed]
- Lee SH, You HJ, Lee YH, Kim DW. Dual vascular free transverse rectus abdominis myocutaneous flap for hemifacial reconstruction in a vessel-depleted neck. Arch Plast Surg 2020;47(1):88-91.
[Crossref] [Google Scholar] [PubMed]
- Han D, Liu W, Li G, Liu L. Circ_PRKDC knockdown promotes skin wound healing by enhancing keratinocyte migration via miR-31/FBN1 axis. J Mol Histol 2021;52(4):681-91.
[Crossref] [Google Scholar] [PubMed]
- Jia YC, Qiu S, Xu J, Kang QL, Chai YM. Docosahexaenoic acid improves diabetic wound healing in a rat model by restoring impaired plasticity of macrophage progenitor cells. Plast Reconstr Surg 2020;145(5):942e-50e.
[Crossref] [Google Scholar] [PubMed]
- Wagner MJ, Cranmer LD, Loggers ET, Pollack SM. Propranolol for the treatment of vascular sarcomas. J Exp Pharmacol 2018;10:51-8.
[Crossref] [Google Scholar] [PubMed]
- Oda Y, Furukawa H, Murao N, Takakuwa E. Lipofibromatosis arising in an infantile back: A case report. Skin Cancer 2019;33(3):250-4.
- Siegel DH. PHACE syndrome: Infantile hemangiomas associated with multiple congenital anomalies: Clues to the cause. Am J Med Genet C Semin Med Genet 2018;178(4):407-13.
[Crossref] [Google Scholar] [PubMed]
- Zhang H, Wei T, Johnson A, Sun R, Richter G, Strub GM. NOTCH pathway activation in infantile hemangiomas. J Vasc Surg Venous Lymphat Disord 2021;9(2):489-96.
[Crossref] [Google Scholar] [PubMed]
- Lahrichi A, Hali F, Baline K, El Fatoiki FZ, Chiheb S, Khadir K. Effects of propranolol therapy in Moroccan children with infantile hemangioma. Arch Pediatr 2018;25(8):449-51.
[Crossref] [Google Scholar] [PubMed]
- Adams DM, Ricci KW. Infantile hemangiomas in the head and neck region. Otolaryngol Clin North Am 2018;51(1):77-87.
[Crossref] [Google Scholar] [PubMed]
- Parikh A, Driscoll CA, Crowley H, York T, Dachy G, Demoulin JB, et al. Diagnostic limitations and considerations in the imaging evaluation of advanced multicentric infantile myofibromatosis. Radiol Case Rep 2020;15(11):2440-4.
[Crossref] [Google Scholar] [PubMed]

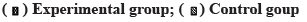
 (b) Statistics of follow-up functional recovery of patients,
(b) Statistics of follow-up functional recovery of patients,