- *Corresponding Author:
- H. J. Dong
Department of Otolaryngology, Zhangjiagang TCM Hospital Affiliated to Nanjing University of Chinese Medicine, No. 77 Changan South Road, Zhangjiagang, Suzhou, Jiangsu 215600, China
E-mail: dhjzyy12345@sina.com
| This article was originally published in a special issue, “Clinical Research in Pharmaceutical and Biomedical Sciences” |
| Indian J Pharm Sci 2021:83(1)Spl issue1;31-36 |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
To investigate the therapeutic effect of transoral laser surgery in patients with early-stage glottic laryngeal cancer. 72 patients were randomly divided into an observation group (n=36) and a control group (n=36), who were diagnosed with early stage portal laryngeal carcinoma by pathological biopsy in our hospital from May 2017 to November 2019. The control group underwent conventional laryngectomy, while the observation group underwent carbon dioxide laser treatment under microscopic supported laryngoscopy. The patients’ treatment status and complications during the 6 mo postoperative follow-up period were also recorded. The results showed that 30 patients in the observation group and 6 patients in the control group had vocal cord neovascularization 6 mo after surgery and 20 patients in the control group had vocal cord neovascularization and 16 patients in the control group had vocal cord neovascularization. There were no statistically significant differences in the preoperative levels of vascular endothelial growth factor, Nitric oxide and tumor necrosis factor-alpha between the two groups (p>0.05), while the postoperative levels of vascular endothelial growth factor, Nitric oxide and tumor necrosis factor-alpha were statistically significant (p<0.05). The effective rate of treatment in the observation group was significantly higher than that in the control group, and the complication rate was lower than that in the control group (p<0.05). The application of micro-supported laryngoscopic carbon dioxide laser for the treatment of early glottic laryngeal carcinoma can improve the clinical treatment effect and reduce postoperative complications, which is worthy of application.
Keywords
Early glottic laryngeal carcinoma, CO2 laser therapy, supported laryngoscope, therapeutic effect
Early glottic carcinoma is a common type of laryngeal carcinoma, which is limited to glottic tissue, does not invade surrounding muscle and cartilage, and does not appear lymph node metastasis. Its pathogenesis is complex, which is considered to be the result of multiple factors, including smoking, drinking, occupation, air pollution, trace elements and sex hormone deficiency. Not timely treatment will not only affect the quality of daily life and work of patients, but also threaten their life safety[1]. Therefore, early diagnosis and treatment is particularly important. Surgical resection is a common treatment for early glottic carcinoma, but surgical resection can easily change the anatomical structure of the larynx, resulting in poor voice quality, difficulty in pronunciation and glottic air leakage, which seriously affects the quality of life of patients[2]. In recent years, with the continuous improvement of surgical instruments such as microscope, laryngoscope and laser, more and more scholars are committed to the study of surgical methods that can completely remove tumor and retain laryngeal function. Transoral laser surgery (TLS) is one of the effective methods to treat some glottic, supraglottic and hypopharyngeal carcinoma[3]. TLS is a microsurgical operation, which can distinguish healthy and diseased tissues, and perform limited resection, while preserving adjacent non diseased tissues. TLS also reduces the need for tracheotomy and nasogastric tube operations. In addition, selecting the right patients can achieve the same oncological results as open surgery[4]. Nevertheless, there are still some deficiencies in TLS. Some studies have reported that although TLS has a relatively low incidence of complications[5], intraoperative and postoperative complications such as bleeding, dyspnea or burning of endotracheal anesthesia intubation may Although rare, airway ignition is also a risk and this particular technique is confined to only early glottic carcinoma[6,7]. Therefore, in this study, we selected 72 cases of early glottic carcinoma as the research object, and analyzed the value and effect of TLS treatment, so as to provide reference for clinical diagnosis and treatment. A total of 72 patients with early glottic carcinoma diagnosed by pathological biopsy in our hospital from May 2017 to November 2019 were included in the study. There were 42 males and 30 females, aged 34-76 (57.25±8.30) y; the course of disease was 3-26 (9.75±2.81) mo; 31 cases were bilateral lesions, 30 cases were unilateral lesions, and 11 cases were located in laryngeal chamber; pathological types: 2 cases of carcinoid, 1 cases of small cell carcinoma, 3 cases of malignant fibrous tissue carcinoma, 5 cases of neuroendocrine carcinoma and 61 cases of squamous cell carcinoma; Tumor nodes metastases (TNM) stage: Carcinoma in situ (Tis) stage 4 cases, Tumor 2 cm or less in greatest dimension (T1) a stage 59 cases, T1b stage 5 cases, Tumor more than 2 cm but not more than 4 cm in greatest dimension (T2) stage 4 cases. They were randomly divided into control group (n=36) and observation group (n=36). The clinical data of the two groups are shown in Table 1. Inclusive criteria: the first diagnosed case; preoperative enhanced computed tomography (CT) examination and fibrolaryngoscope examination showed no lymph node metastasis and thyroid cartilage invasion; no other antitumor treatment; informed of this study and voluntarily signed informed consent.
| Project | Control group | Observation group | t | p |
|---|---|---|---|---|
| Age | 58.37±7.73 | 57.02±9.20 | 1.065 | 0.431 |
| Gender (male/female) | 22/14 | 20/16 | 0.937 | 0.655 |
| Course of disease (mo) | 9.56±1.97 | 9.97±2.23 | 1.156 | 0.237 |
| Types of lesions | 1.368 | 0.097 | ||
| Unilateral lesions | 24 | 27 | ||
| Bilateral lesions | 35 | 32 | ||
| Laryngeal lesions | 6 | 5 | ||
| Pathological type | 0.877 | 0.732 | ||
| Carcinoid | 1 | 1 | ||
| small cell carcinoma | 0 | 1 | ||
| Malignant fibrohistoma | 2 | 1 | ||
| Neuroendocrine tumor | 2 | 3 | ||
| squamous cell carcinoma | 29 | 32 | ||
| TNM stage | 0.903 | 0.571 | ||
| Tis | 3 | 1 | ||
| T1a | 30 | 29 | ||
| T1b | 2 | 3 | ||
| T2 | 2 | 2 |
Table 1: Comparison of General Clinical Data between the Two Groups
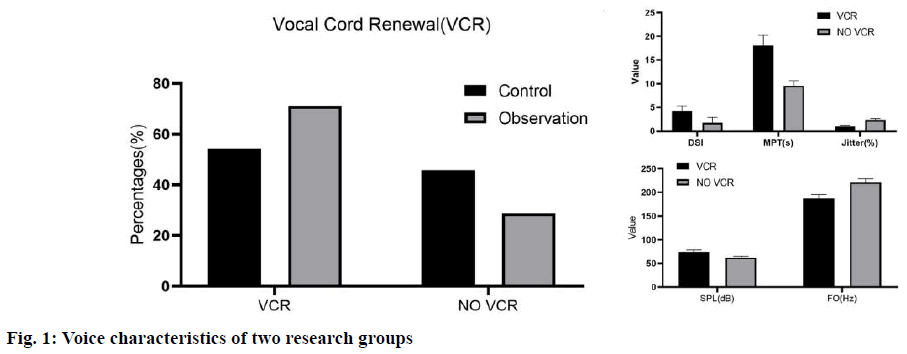
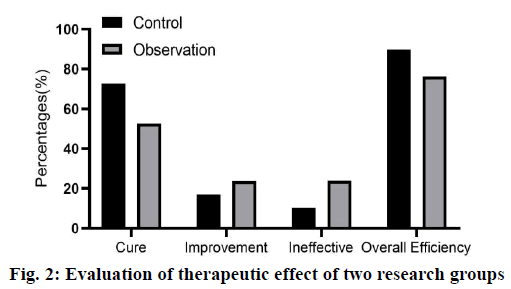
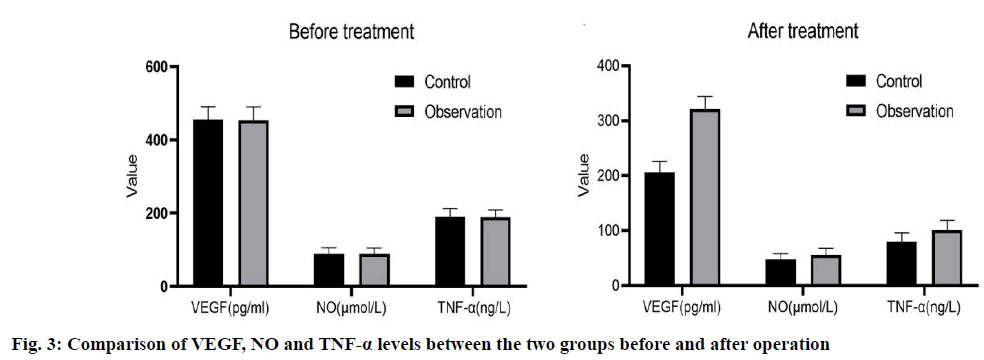
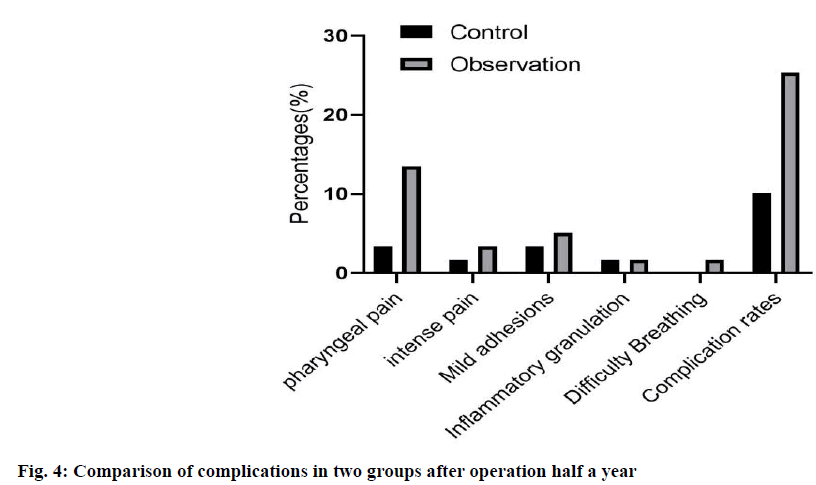
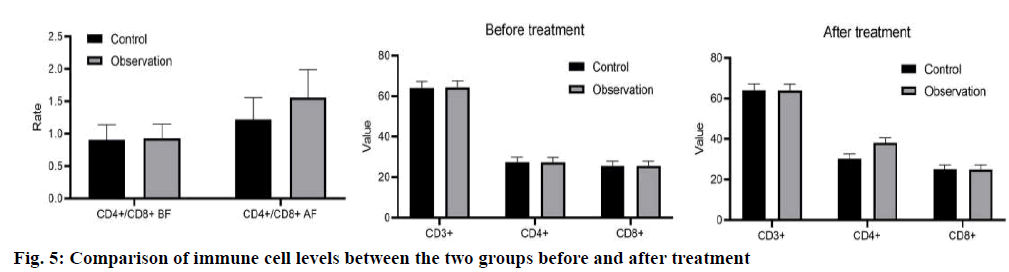
Exclusion criteria: poor tolerance to surgery; age >80 y old; severe liver and kidney dysfunction; coagulation dysfunction; other throat lesions. The study was approved by the hospital ethics committee; all patients agreed and signed informed consent. Control group: all patients received conventional laryngeal split vocal cord resection, local anesthesia and tracheal intubation, and conventional “U” incision was made. After laryngeal split, the tumor size and laryngeal cavity were explored, and the tumor tissue of 0.5~1.0 normal tissue around vocal cord laryngeal cancer was removed. After the operation, the free ventricular zone and subglottic mucosa were sutured with thyroid cartilage plate, and antibiotics were given at the end of the operation. Observation group: TLS treatment was carried out under microscopically supported laryngoscope. The specific methods were as follows: routine laryngoscope and operation microscope were selected. The position of laryngeal tumor was determined by supporting the posterior neck, and the subglottic was cured by the balloon of protective anesthesia catheter. Then, according to the patient’s condition, the microscope display position was adjusted, and the laser power was set at 3~5 W. Continuous output, adjust the focal length of the microscope and the laser focal length, cut the tumor with the help of red laser aiming at the spot, and then use glucocorticoid and antibiotics for anti-infection treatment at the end of the operation.Voice characteristics: 6 mo after surgery, the vocal cord regeneration was observed by fiber laryngoscope and dynamic laryngoscope, and then the voice characteristics of patients were analyzed by divas 2.5 voice analysis software. Dysphonia Severity Index (DSI), Maximum phonation time (MPT), Sound Pressure Level (SPL), Jitter and FO were recorded. The curative effect of the two groups was observed. Cure: the degree of symptom relief was more than 90 % and the laryngeal function was preserved. No recurrence was found after half a year follow-up. Improvement: the degree of remission was 70 %-90 %, the laryngeal function was basically preserved and the recurrence was less during followup. Ineffective: foreign body sensation and discomfort still exist in the throat after operation, and the remission degree is less than 60 %, and the laryngeal function is not reserved, and there is more recurrence in the followup This makes the procedure not applicable to all the stages of glottis carcinoma, but substantially useful to the patients who are diagnosed at earIy stage. Serum Vascular endothelial growth factor (VEGF) and Tumor necrosis factor-alpha (TNF-α) were measured by enzyme-linked immunosorbent assay, and Nitric oxide (NO) was determined by nitrate reductase method. All operation steps were carried out in strict accordance with the instructions of the kit. The incidence of postoperative complications. 6 mo later, the incidence of complications such as conscious pharyngeal pain, conscious strong pain, local mild adhesion, inflammatory granulation tissue hyperplasia and dyspnea were collected. All experiments were repeated at least 3 times, and all data were expressed as mean±SD. The differences between the two groups were analyzed by t-test, and multiple comparisons were performed by one-way ANOVA. p<0.05 was considered statistically significant. In the observation group, 30 cases of vocal cord neogenesis, 6 cases of vocal cord neogenesis, 20 cases of vocal cord neogenesis, 16 cases of vocal cord neogenesis in the control group. The DSI, MPT and SPL levels were higher in the vocal cord newborn patients than those in the vocal cord newborn patients, while the Jitter and FO levels were significantly lower (p<0.05), as shown in fig. 1. As shown in fig. 2, the total effective rate of the observation group (89.83 %) was significantly higher than that of the control group (76.27 %) (p<0.05). As shown in fig. 3, there were statistically significant differences in the levels of VEGF, NO and TNF-α between the two groups (p<0.05). However, there was no significant difference in VEGF, NO and TNF-α levels between the two groups (p>0.05). Compared with the control group, the incidence of complications such as pharyngeal pain, conscious strong pain, local mild adhesion, local mild adhesion, inflammatory granulation tissue hyperplasia and dyspnea in the observation group were significantly lower than those in the observation group (p<0.05) as shown in fig. 4. The levels of cluster of differentiation (CD) CD4+ and CD4+/CD8+ in the observation group were significantly higher than that in the control group (p<0.05), While there was no significant difference in the levels of CD3+, CD8+ before and after treatment (p>0.05); and was no significant difference in CD4+ and CD4+/CD8+ levels before and after treatment in the two groups (p>0.05), as shown in fig. 5. Glottic carcinoma has typical clinical manifestations in the early stage, and the degree of pathological differentiation and diagnostic accuracy are high. In general, standardized treatment after diagnosis can ensure that the 5 y survival rate increases to more than 90 %[8]. Previous clinical manifestations showed that the patient had dysphagia or foreign body sensation in the throat for more than 1 mo, and the patient was 40-50 y old. In addition, in addition to the above symptoms, throat pain, bloody sputum and other symptoms are also the basis for early diagnosis of glottic carcinoma[9]. Traditional vocal cord resection is traumatic, can cause greater pain to patients, but also hinder their postoperative recovery. TLS is a new surgical treatment method[10]. The use of laryngoscope can accurately show the location of laryngeal lesions, and TLS can complete the cutting and coagulation of lesions, while the use of microscope can enlarge the surgical field, which can improve the treatment accuracy and reduce the damage to surrounding tissues. Our results showed that DSI, MPT and SPL levels in patients with vocal cord regeneration were significantly higher than those in patients with vocal cord regeneration, while jitter and FO levels were lower, indicating that TLS is helpful to vocal cord regeneration and restore voice characteristics. Previous studies have found that the application of TLS in the treatment of early glottic carcinoma can shorten the postoperative recovery time, improve the clinical operation effect and reduce the incidence of complications[11]. In addition, the use of TLS in the treatment of glottic carcinoma has a low recurrence rate, no serious complications, and high long-term survival rate[12]. The results of this study showed that the total effective rate of the observation group was higher than that of the control group, and the incidence of complications was lower than that of the control group, which was basically consistent with the above research results, which further demonstrated the effectiveness and safety of TLS treatment. No, as an effector molecule of anti-tumor, has been proved to promote tumor growth at low concentration and promote tumor cell death at high concentration[13]. Many follow-up studies have shown that serum levels are closely related to the occurrence, development and prognosis of tumors[14]. VEGF is another important angiogenic factor. In the research field of early glottic carcinoma, VEGF is also closely related to the induction of tumor angiogenesis[15,16], lymphangiogenesis and tumor lymph node metastasis[17]. The main source of VEGF secretion in tumor patients is tumor cells, its high level expression can be seen in tumor tissue and serum and there is a positive correlation between them[18]. Some studies have pointed out that serum VEGF level can be used as an auxiliary reference index to judge the benign and malignant laryngeal diseases and prognosis[19]. TNF-α is a cytokine secreted by activated macrophages, which has many biological effects such as immune response, anti-infection and promoting cell growth and differentiation[20]. Studies have shown that TNF-α also has antitumor effects by inhibiting tumor growth and other mechanisms[21]. In addition, we detected the immune cell levels of the two groups before and after treatment and found that after treatment, CD4+ and The level of CD4+/CD8+ in the treatment group was significantly higher than that in the control group (p<0.05), indicating that TLS treatment can inhibit the body’s excessive inflammatory response, minimize the risk of multiple organ injury, help to regulate the immune level of the body and fundamentally achieve the purpose of disease treatment. After treatment, the levels of VEGF, NO and TNF-α in the two groups decreased compared with those before treatment and the indexes can be used as the reference standard to judge the curative effect. Conclusion: TLS combined with PRA is more effective in reducing serum VEGF, NO and TNF-α level in patients with early glottic carcinoma. This may be due to the fact that TLS combined with PRA preserves the laryngeal function as much as possible, so that the serum levels of VEGF, NO and TNF-α related to prognosis are lower than those in the traditional operation group, but the specific mechanism still needs to be further explored. In conclusion, TLS is effective and safe in the treatment of early glottic carcinoma, which is worthy of clinical application.
Conflicts of interest:
The authors report no conflicts of interest.
Acknowledgements:
This work was supported by the Special Technology for Diagnosis and Treatment of Key Clinical Diseases in Suzhou (NO. LCZX201723).
References
- Preuss SF, Cramer K, Klussmann JP, Eckel HE, Guntinas-Lichius O. Transoral laser surgery for laryngeal cancer: outcome, complications and prognostic factors in 275 patients. Eur J Surg Oncol 2009;35:235-40.
- Gal S, Ramirez JI, Maguina P. Autologous fat grafting does not improve burn scar appearance: a prospective, randomized, double-blinded, placebo-controlled, pilot study. Burns 2017;43:486-9.
- De Bonnecaze G, Vairel B, Dupret-Bories A, Serrano E, Vergez S. Transoral robotic surgery of the tongue base for obstructive sleep apnea: Preliminary results. Eur Ann Otorhinolaryngol Head Neck Dis 2018;135:411-5.
- Motta G, Esposito E, Motta S, Tartaro G, Testa D. CO2 laser surgery in the treatment of glottic cancer. Head Neck 2005;27:566-74.
- Cabanillas R, Rodrigo JP, Llorente JL, Suárez V, Ortega P, Suárez C. Functional outcomes of transoral laser surgery of supraglottic carcinoma compared with a transcervical approach. Head Neck 2004;26:653-9.
- Tlemsani C, Mir O, Psimaras D, Vano YA, Ducreux M, Escudier B, et al. Acute neurovascular events in cancer patients receiving anti-vascular endothelial growth factor agents: Clinical experience in Paris University Hospitals. Eur J Cancer 2016;66:75-82.
- Lee SW, Markham PF, Markham JF, Petermann I, Noormohammadi AH, Browning GF, et al. First complete genome sequence of infectious laryngotracheitis virus. BMC genomics 2011;12:1-6.
- Balkwill F. Tumor necrosis factor and cancer. Nat Rev Cancer 2009;9:361-71.
- Vilaseca‐González I, Bernal‐Sprekelsen M, Blanch‐Alejandro JL, Moragas‐Lluis M. Complications in transoral CO2 laser surgery for carcinoma of the larynx and hypopharynx. Head Neck 2003;25:382-8.
- Sigston E, De Mones E, Babin E, Hans S, Hartl DM, Clement P, et al. Early-stage glottic cancer: oncological results and margins in laser cordectomy. Arch Otolaryngol Head Neck Surg 2006;132:147-52.
- Rebeiz EE, Wang Z, McGilligan JA, Annino DJ, Shapshay SM. Preliminary clinical results of window partial laryngectomy: a combined endoscopic and open technique. Ann Otol Rhinol Laryngol 2000;109:123-7.
- Lombardo N, Aragona T, Alsayyad S, Pelaia G, Terracciano R, Savino R. Objective and self-evaluation voice analysis after transoral laser cordectomy and radiotherapy in T1a-T1b glottic cancer. Lasers Med Sci 2018;33:141-7.
- Crespo AN, Chone CT, Gripp FM, Spina AL, Altemani A. Role of margin status in recurrence after CO2 laser endoscopic resection of early glottic cancer. Acta Otolaryngol 2006;126:306-10.
- Pfister DG, Laurie SA, Weinstein GS, Mendenhall WM, Adelstein DJ, Ang KK, et al. American Society of Clinical Oncology clinical practice guideline for the use of larynx-preservation strategies in the treatment of laryngeal cancer. J Clin Oncol 2006;24:3693-704.
- Jeong WJ, Kim H, Ahn JC, Sung MW, Kim KH, Ahn SH. Serial endoscopic analysis of the glottis following laser cordectomy: from an oncological perspective. Lasers Med Sci 2012;27:1025-31.
- Steiner W, Ambrosch P, Rödel RM, Kron M. Impact of anterior commissure involvement on local control of early glottic carcinoma treated by laser microresection. Laryngoscope 2004;114:1485-91.
- Comert E, Tunçel U, Dizman A, Yukselen Guney Y. Comparison of early oncological results of diode laser surgery with radiotherapy for early glottic carcinoma. Otolaryngol Head Neck Surg 2014;150:818-23.
- Fang TJ, Courey MS, Liao CT, Yen TC, Li HY. Frozen margin analysis as a prognosis predictor in early glottic cancer by laser cordectomy. Laryngoscope. 2013;123:1490-5.
- Michel J, Fakhry N, Duflo S, Lagier A, Mancini J, Dessi P, et al. Prognostic value of the status of resection margins after endoscopic laser cordectomy for T1a glottic carcinoma. Eur Ann Otorhinolaryngol Head Neck Dis 2011;128:297-300.
- Brøndbo K, Fridrich K, Boysen M. Laser surgery of T 1a glottic carcinomas; significance of resection margins. Eur Arch Otorhinolaryngol 2007;264:627-30.
- Chu PY, Hsu YB, Lee TL, Fu S, Wang LM, Kao YC. Longitudinal analysis of voice quality in patients with early glottic cancer after transoral laser microsurgery. Head Neck 2012;34:1294-8.