- *Corresponding Author:
- Y. Liu
Suzhou Eye Hospital, Suzhou, Jiangsu 215000, China
E-mail: 2739681831@qq.com
| This article was originally published in a special issue, "Clinical and Experimental Studies on Drug and Intervention Repurposing in China |
| Indian J Pharm Sci 2019:81(4)spl issue1;35-40 |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
The incidence of myopia is increasing especially in teenagers, therefore the widespread technology, orthokeratology is worthy discussing. This article describes eye vision and the shape of the cornea on the basis of topography check and Fourier analysis model in clinical application treated with orthokeratology for one year. All patients underwent ophthalmic examination to exclude ocular disease and contraindications to lens. And the all patients received orthokeratology at night with corneal plastic glasses. The uncorrected visual acuity and optometry were examined, and the mean curvature of the anterior and posterior surfaces of the cornea were also measured to obtain the Fourier index each time in the Fourier analysis. After orthokeratology for one year, we found that the position of the thinnest cornea was not significantly shifted. But Fourier analysis shows that corneal plasticizer has different correction effects on minimum spherical radius and spherical eccentricity, as well as peripheral regular astigmatism and center regular astigmatism, which may be one of the main reasons to alleviate the development of myopia.
Keywords
Fourier analysis, juvenile myopia, corneal surface morphology
Orthokeratology is a kind of rigid contact lens with high oxygen permeability designed based on the personalized shape of human cornea. It reshapes the shape of the front surface of the cornea at night to change the corneal diopter, so as to obtain normal naked eye vision during the day[1]. Besides, it has the effect of delaying the development of myopia which is helpful to achieve myopia correction. Orthokeratology as a non-surgical correction of myopia, a variety of new lens design and the emergence of advanced CNC machining technology can be achieved to produce a variety of complex curved optical lenses with the development of a large number of high-permeability materials[2]. In addition, the speed, efficacy, stability and safety of corneal plastic lens in reducing diopter are significantly improved than before, especially can slow down the development of adolescent myopia.
Whether in China or in the world, the incidence of myopia is increasing year by year, and it is becoming younger and younger. In recent years, more and more cases of myopia among adolescents and even younger children is becoming common. Statistics from the ministry of education show that the trend of low age of Chinese students with poor eyesight is obvious, and the myopia of primary school students has doubled in 10 y[3]. A research report of the world health organization showed that there are 600 million myopia patients in China, and the myopia rate among teenagers of China ranks first in the world. The myopia rate of high school students and college students has exceeded 70 % and has increased year by year. And as prediction, by 2050, the global prevalence of myopia will reach 52 %. Myopia besides congenital genetic element outside, the lifestyle at ordinary times, especially outdoor activity is insufficient[4-6]. Another factor is that the overburden of studies can aggravate myopia. In addition, the frequent use of tablet computers, smart phones and other electronic products has increased the probability of myopia of children. Myopia causes vision loss and related complications, which seriously affect the physical and mental health of teenagers. With the progressive deepening of myopia, the harm of high myopia directly hinders the learning, sports and life quality of teenagers, and has become a social problem troubling countless students and parents[7]. High myopia is a high risk factor for severe vision loss or impaired visual function which can be irreversible.
In recent years, the application of orthokeratology has made great progress in the study of optical mass of the eyeball and the biomechanics of the cornea. Although orthokeratology is widely used in China, there is no uniform regulation on the content and preoperative and postoperative examination is limited. The conventional analysis model and parameters have some limitations, and the corneal topography is an essential examination content for the examination and reexamination. This research will be based on the corneal topography check and Fourier analysis model is introduced into the shape of the cornea in clinical application. It is designed to have the objective and correct evaluation of orthokeratology and prevent possible mechanism in the adolescent myopia development and application in clinical effect.
Materials and Methods
Objective of the study:
All the data are from the clinical research in August 2016 to December. Myopia patients with orthokeratology and no other eye or systemic diseases, which can cause eye lesions in patients were included in the study. The total number of myopia patients selected into the study was 40 (80 eyes), including 25 male (50 eyes) and 15 female (30 eyes). The age range is from 8 to 23 y and the average age is 14.1±0.56 y. The average equivalent spherical mirror scope is –2.86±0.94 D. The follow-up period was 12 mo, with a total of 7 visits.
Material and equipment:
The lens used in this study was a Boston Equalens II high-oxygen permeable lens with a Dk value (oxygen permeable index) of at least 90×10-11 (cm2·ml O2/s·ml·hPa). The lens diameter was 10-11 mm and the thickness of the central optical center was 0.22 mm. A shaping mirror is designed for the traditional four arc region inverse geometry, which is composed of central optical region, reverse arc region, peripheral positioning arc region and peripheral arc region. In addition, other materials and equipment include: eye drops, standard eye chart, contact-free tonometer, fluorescein sodium ophthalmic test paper, slit lamp microscope, optometry test kit, corneal topography tester and so on.
Test method:
At first, the patients were examined by slit lamp microscope before the orthokeratology and the pathological changes of anterior ganglia if any were excluded. Then a tonometer was used to measure the intraocular pressure and abnormal conditions such as high intraocular pressure were eliminated. In addition, comprehensive optometry was performed to exclude patients with corrected vision less than 1.0. The data were recorded and the eligible patients were screened. For patients meeting the requirements, eye drops were used for mydriasis and optometry once every 5 min for a total of five times. The degree of spherical mirror and column mirror before wearing glasses were obtained and then the equivalent spherical mirror degree was calculated.
After preparation, the fitting of orthokeratology was performed. The processes were as follows, standard plate test method was adopted, and a complete set of standard lens boxes designed by the manufacturer was adopted. According to the expected diopter reduction of the patient and the examination results of corneal topography, a trial piece was selected from the standard lens by the fitting technician.
The parameters were determined according to the position, range of motion and vision of the glasses when fitting. The procedure of wearing glasses usually requires 2 h of observation, and at the end of the trial, the naked eye vision and topographic map are checked to understand the reduction and positioning.
The position and activity of the lens were observed under the cobalt blue light of the slit lamp. The lens was adjusted according to the patient's condition, because the ideal lens fit requires the lens to have good center positioning, the range of motion of the lens is 0.5~1.0mm when blinking. Fluorescein examination showed that there was no fluorescence in the central base arc region, while the reversed arc region was a wide fluorescence filling region. After selecting the ideal adaptor, the prescription of the adaptor was determined and the lens were customize. All patients were fitted with a corneal plastic lens at night for more than 7 h each night.
Follow-up arrangements were then made before fitting and 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y after fitting with the lens. A total of 7 times were on-going. During the follow-up, basic examinations were required, including the patient's subjective feeling of wearing the glasses and the slit lamp's examination of wearing the glasses. The conjunctiva and the lens were also examined after removal. Noncontact intraocular pressure was measured postoperatively. The corneal topography was used to check corneal shaping, corneal morphological changes, and whether the optical region was out of alignment.
Fourier analysis:
The conversion of periodic curves to Fourier harmonic components is widely used in electrical and biomedical engineering. Fourier analysis is also used to precisely simulate the polarity changes in view power values. The trigonometric form of the Fourier series for periodic signals[8,9] was, Eqn. 1, x(t)=x(t+T)=x(t+2T)=x(t+3T)=..=x(t+nT), where, n=±1, ±2, ±3,…; and T is the period. The trigonometric expansion for the Fourier series was, Eqn. 2, x(t)=a0+Σn=1(an cos nw0t+bn sin nw0t), where, n=1, 2, 3,… And the Fourier series were, Eqn. 3, a0=1/T ∫T/2–T/2 x(t)dt; Eqn. 4, an=2/T ∫T/2 –T/2 x(t) cos nw0tdt; Eqn. 5, bn=2/T ∫T/2 –T/2 x(t) sin nw0tdt, where n=1, 2, 3,; ω0 is the fundamental frequency and equals 2π/T; T is period.
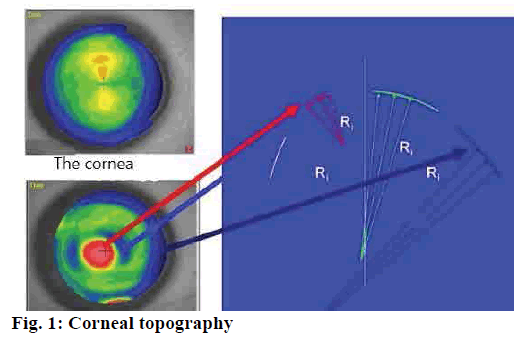
Fourier map topographic analysis means performing Fourier analysis on the refractive force of each detection point obtained by Maya image analysis within a region with a diameter of 3 mm (1 to 9 rings) to 6 mm (1 to 20 rings). At the bottom, as shown in fig. 1 below, is a corneal topography map, with red for bumps, green for flatter areas, and blue for sea level (lower), showing an irregular cornea. The corneal shape shown by the color coding diagram in the corneal topographic map is a qualitative and intuitive expression of the corneal refractive state, while the most commonly used quantitative parameters are simulated kerotoscope reading, minimum keratoscope reading, surface regularity index and surface asymmetric index. The simuIafed kerotoscope reading and minimum keratoscope reading are according to the image on the cornea 7, 8, 9 ring axial diopter data derived. Usually 7, 8, 9 ring corresponding corneal surface diameter of about 3 mm to 4 mm, corresponding to the central region of the cornea. However, surface regularity index is expressed for performance center ring 5 which is corresponding to the diameter of about 2 mm. surface regularity index describes the degree of regularity of corneal pupil area according to the data analysis of ring 1-10.
The processes were as follows, the uncorrected views, the refractive index and the spherical refractive index were recorded at each follow-up time point, and the equivalent spherical refractive index was calculated. The mean curvature, corneal astigmatism and Q values of the front and rear surfaces of the cornea were obtained according to the data measured in the anterior segment, and the corneal thickness at the vertex, the thinnest point and the thinnest point coordinates (x, y) were obtained. Calculate the distance between the thinnest point and the vertex according to the coordinates. The Fourier indices in the Fourier analysis are obtained from the data measured in the anterior segment. The 0 index refers to the spherical part, the first index corresponds to the asymmetric part, the second index refers to the astigmatism part, and the Fourier index up to the third degree refers to the higher-order irregular astigmatism.
Statistical processing:
SPSS 19.0 statistical software package was used and paired sample t test was performed. Data are expressed as mean±standard deviation except Special instructions. P<0.05 was considered statistically significant. F test was used for homogeneity of variance, and t test was used for heterogeneity of variance.
Results and Discussion
The orthokeratology was studied in 40 patients with patients. The results showed that during the follow-up, lens problems occurred in 7 patients, but all lenses were replaced within 1 w. During the follow-up, none of the 40 patients were found to have severe lesions of the anterior surface space under the slit lamp examination. Eight patients showed slight epithelium loss within 3 mo after orthokeratology and continued to participate in the study after the treatment with eye drops.
All patients showed significant improvement in naked eye vision during the 1-y follow-up as shown in Table 1. Mean value of naked eye vision were, 4.15±0.12, 4.56±0.21, 4.85±0.08, 4.96±0.02, 4.99±0.15, 5.00±0.02, 5.20±0.03 before orthokeratology and after for 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y. There were statistically significant differences between each group and the pre-lens group (p<0.05). The patients in this study had been wearing glasses for about 1 mo, and the visual acuity of the naked eyes was basically normal, reaching more than 4.9. Therefore, naked eye vision examination is one of the important indexes to evaluate the curative effect of orthokeratology[10]. Orthokeratology can provide good UCVA, which can meet the day vision needs of wearers as discussed in literature.
| Follow-up time | Eye Number | Mean±SD |
|---|---|---|
| Before orthokeratology | 80 | -2.90±0.56D |
| One day | 80 | -2.05±0.67D |
| One week, | 80 | -1.07±0.94D |
| One month, | 80 | -0.34±0.56D |
| Three months, | 80 | -0.15±0.34D |
| Six months | 80 | -0.08±0.69D |
| One year | 80 | -0.19±0.35D |
Note: In the follow-up of one week, p<0.0001; one week to one month, p<0.05; after one month p>0.05
Table 1: Spherical equivalent degree before and after wearing glasses (X±S)
The decrease of myopia degree and flattening of corneal curvature are the key parameters to evaluate the effect of corneal shaping mirror. As shown in Table 2, the spherical equivalent degree has been decreased significantly. Mean value of spherical equivalent degree were, -2.90±0.56D, -2.05±0.67D, -1.07±0.94D, -0.34±0.56D, -0.15±0.34D, -0.08±0.69D, -0.19±0.35D after orthokeratology 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y. Compared to the before wearing the lens, the equivalent spherical degree was significantly reduced, which decreased significantly in the first week and slowly from 1 w to 1 mo. And after 1 mo, the spherical equivalent degree reached stability.
| Follow-up time | Eye Number | Mean±SD | Increase±SD |
|---|---|---|---|
| Before orthokeratology | 80 | 4.15±0.12 | -- |
| One day | 80 | 4.56±0.21 | 0.32±0.11 |
| One week, | 80 | 4.85±0.08 | 0.57±0.21 |
| One month, | 80 | 4.96±0.02 | 0.58±0.25 |
| Three months, | 80 | 4.99±0.15 | 0.76±0.24 |
| Six months | 80 | 5.00±0.02 | 0.70±0.22 |
| One year | 80 | 4.99±0.01 | 0.65±0.24 |
Note: In the follow-up, visual acuity after orthokeratology compared with before orthokeratology, p<0.05
Table 2: Uncorrected visual acuity eyes before and after wearing glasses (X±S)
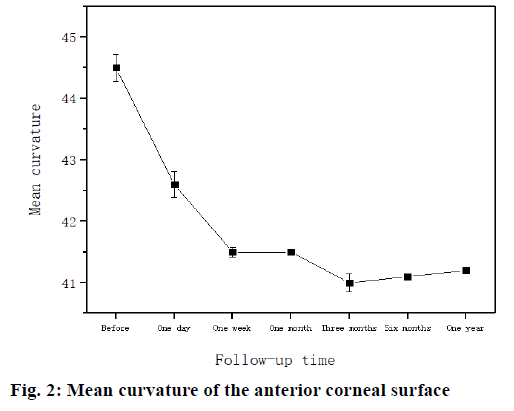
The mean curvature of the anterior corneal surface has decreased. Mean value of Mean curvature of the anterior corneal surface were 44.5±0.22D, 42.6±0.21, 41.5±0.08, 41.0±0.02, 41.1±0.15, 41.0±0.02, 41.2±0.03. The decreased trend is displayed in fig. 2.
The mean curvature of the anterior surface of the cornea decreased compared with that before the orthokeratology. Within 1 w after wearing the glasses, all of them decreased significantly. There was no significant difference between the two groups, and the curvature increased slightly (p>0.05) after 3 mo. The quantitative changes of spherical curvature objectively show the theoretical basis for the flattening of the central cornea and the relative steepening of the central cornea after orthokeratology, which provides a theoretical basis for the explanation of the mechanism of peripheral myopia drift and the reduction of peripheral hyperopia defocusing caused by corneal plastic surgery, namely correction of central refractive error.
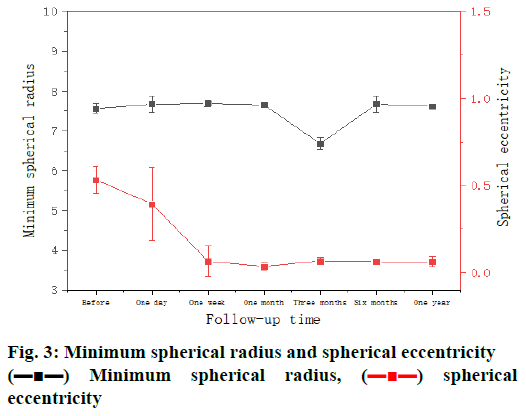
So far, there are 2 main theories about the mechanism of temporarily reduce mean curvature. A school of thought is that corneal shape played a major role in corneal surface before orthokeratology, and has little after corneal surface forces. However, another theory is that the corneal shape not only acts on the corneal surface before orthokeratology, but also acts on the surface after orthokeratology by pressing the cornea achieve the goal of lower diopter. Although the above results show the changes of corneal curvature, they do not reflect the differences of corneal morphological changes caused by different arcs of the corneal shaping mirror[11]. Therefore, Fourier analysis was employed to measure the parameters of different regions of the cornea, in order to find the theoretical basis to explain the mechanism of orthokeratology. The minimum spherical radii were 7.56±0.12, 7.67±0.21, 7.69±0.08, 7.65±0.02, 6.68±0.15, 7.67±0.20, 7.62±0.03 mm before orthokeratology and after for 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y. Fig. 3 shows a changed trend. Compared with the situation before orthokeratology, the minimum spherical radius increased after orthokeratology for 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y.
The spherical eccentricity were 0.553±0.075, 0.395±0.211, 0.065±0.087, 0.036±0.022, 0.068±0.190, 0.063±0.010, 0.062±0.030 before orthokeratology and after for 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y. Compared with the situation before orthokeratology, the minimum spherical radius decreased after orthokeratology for one day, one week, one month, three months, six months and one year. Great decrease showed in one week and after that spherical eccentricity was stable. But the lowest spherical eccentricity was reached in one month. These results were illustrated in fig. 3.
Before orthokeratology, the 3-mm area asymmetry was 0.23±0.12, and the 6-mm area asymmetric was 0.33±0.10. In the follow-up observation, 3-mm and 6-mm area asymmetric were 0.50±0.26, 0.63±0.33, respectively for 1 d after orthokeratology. For 1 w after orthokeratology, 3-mm and 6-mm area asymmetric were 0.60±0.25, 0.73±0.23, respectively. For 1 mo after orthokeratology, 3-mm and 6-mm area asymmetric were 0.58±0.25, 0.36±0.23, respectively. The detailed results were shown in Table 3.
| Follow-up time | Eye Number | 3-mm | 6-mm |
|---|---|---|---|
| Before orthokeratology | 80 | 0.23±0.12 | 0.33±0.10 |
| One day | 80 | 0.50±0.26 | 0.63±0.33 |
| One week, | 80 | 0.60±0.25 | 0.73±0.23 |
| One month, | 80 | 0.58±0.25 | 0.36±0.23 |
| Three months, | 80 | 0.57±0.15 | 0.88±0.21 |
| Six months | 80 | 0.56±0.15 | 0.85±0.18 |
| One year | 80 | 0.58±0.15 | 0.78±0.11 |
Table 3: Comparison of asymmetric part before and after orthokeratology (X±S)
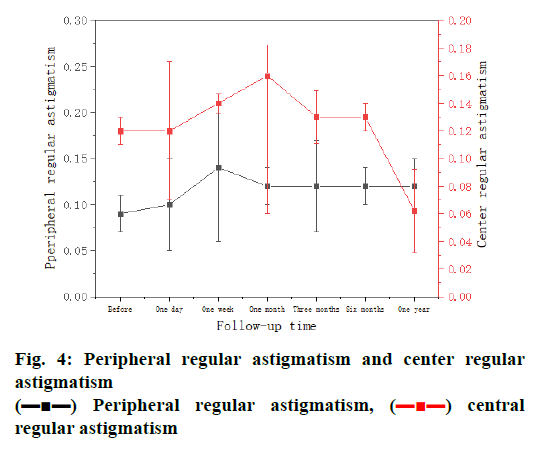
The peripheral regular astigmatism were 0.09±0.12, 0.10±0.21, 0.11±0.08, 0.14±0.02, 0.12±0.15, 0.12±0.20, 0.12±0.03 before orthokeratology and after for 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y. Fig. 4 shows the changed trend. Peripheral regular astigmatism increased after 1 d orthokeratology, but the Statistical significance is none (p=0.60). In addition, the center regular astigmatism was also evaluated as shown in fig. 4. The entire trend is increasing and for 1 mo, the increase was large.
The higher-order irregular were 0.019±0.002, 0.020±0.010, 0.024±0.008, 0.034±0.02, 0.028±0.015, 0.03±0.002, 0.029±0.019 before orthokeratology and after 1 d, 1 w, 1 mo, 3 mo, 6 mo and 1 y. The detailed results were shown in Table 4.
| Follow-up time | Eye Number | Higher-order irregular astigmatism |
|---|---|---|
| Before orthokeratology | 80 | 0.019±0.002 |
| One day | 80 | 0.020±0.010 |
| One week, | 80 | 0.024±0.008 |
| One month, | 80 | 0.034±0.02 |
| Three months, | 80 | 0.028±0.015 |
| Six months | 80 | 0.03±0.002 |
| One year | 80 | 0.029±0.019 |
Table 4: Comparison of higher-order part before and after orthokeratology (X±S)
This study analysed the visual acuity and corneal examination before and after orthokeratology through clinical observation. The changes of the anterior and posterior surfaces of the cornea confirmed that the refractive correction of myopia by orthokeratology was achieved by flattening the anterior surface of the cornea and reducing the curvature of the cornea, but the effect on the posterior surface of the cornea was not obvious. Such changes were significantly changed within 1 mo after wearing the lens, and tended to be stable after wearing the lens for 1 mo. After 1 y of corneal plastic surgery, it was found that the corneal thickness was not significantly affected by the orthokeratology, and the position of the thinnest cornea was not significantly shifted. Besides, orthokeratology had a significant effect on all the parameters of the Fourier analysis, and the change was obvious after orthokeratology for 1 mo. Fourier analysis can be used as a way to evaluate the influence of the orthokeratology on the optical characteristics of the cornea. In addition, Fourier analysis shows that corneal plasticizer has different correction effects on central and peripheral corneal refractive errors, which may be one of the main reasons to alleviate the development of myopia.
References
- Jing Z. A Pilot Study of SMILE for Hyperopia: Corneal Morphology and Surface Characteristics of Concave Lenticules in Human Donor Eyes. J Refract Surg 2016;32(10):713-6.
- Stach S, Ţălu Ş, Trabattoni S, Tavazzi S, Głuchaczka A, Siek P, et al. Morphological properties of siloxane-hydrogel contact lens surfaces. Curr Eye Res 2017;42(4):498-505.
- Bin Z, Li W, He W. Therapeutic efficiency of sodium hyaluronate eye drops on dry eye in juvenile with myopia wearing rigid gas permeable contact lens. Guoji Yanke Zazhi 2016;16(3):511-3.
- Greene PR, Medina A. Juvenile Myopia. Predicting the Progression Rate. Mathews J Ophthalmol 2017;2(1):012.
- Yu-Min L. Clinical effect of the midperipherv additional designed lenses combined adjustment training on myopia in childhood. Guoji Yanke Zazhi 2015;15(11):1960-3.
- Xia L, Zhang MJ, Song XS. Observation on the long-term effectiveness and safety of juvenile myopia patients wearing orthokeratology. Guoji Yanke Zazhi 2018;18(5):968-70.
- Jing X. Regression analysis on influence factors of orthokeratology controlling juvenile myopia progression. Guoji Yanke Zazhi 2015;15(5):872-4.
- Fourier analysis by Weller H. 2015. Available from: http://www.met.reading.ac.uk/~sws02hs/teaching/Fourier/Fourier_2_student.pdf.
- Mingo-Botín D, Arnalich-Montiel F, Couceiro de Juan A, Ortiz-Toquero S. Repeatability and Intersession Reproducibility of Pentacam Corneal Thickness Maps in Fuchs Dystrophy and Endothelial orthokeratology. Cornea 2018;37(8): 987-92.
- Edward L, Golebiowski B, Swarbrick HA. Changes in corneal subbasal nerve morphology and sensitivity during orthokeratology: onset of change. Ocul Surf 2017;15(2):227-35.
- Woreta FA, Davis GW, Bower KS. LASIK and surface ablation in corneal dystrophies. Surv Ophthalmol 2015;60(2):115-22.
 Minimum spherical radius,
Minimum spherical radius,  spherical eccentricity
spherical eccentricity