- *Corresponding Author:
- R. Guo
Institute of Clinical Pharmacology, Qilu Hospital of Shandong University, Jinan, China
E-mail: grc7636@126.com
| Date of Submission | 14 October 2016 |
| Date of Revision | 07 April 2017 |
| Date of Acceptance | 13 October 2017 |
| Indian J Pharm Sci 2017;79(6): 1025-1029 |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
Carbamazepine is one of the most frequently prescribed antiepileptic drugs and influence of genetic differences, sex, age and race on the plasma levels of carbamazepine and its metabolites is well known. The objective of this study was to assess and compare the compliance, safety and toxicity in different age and gender groups of Chinese epileptic patients on the basis of therapeutic drug monitoring results of carbamazepine, since Han-Chinese are at higher risk of developing serious and fatal adverse effects when exposed to carbamazepine. The therapeutic drug monitoring results of carbamazepine in epileptic patients, obtained with validated methods were complied, evaluated and compared for compliance, safety and toxicity in different age and gender groups of Chinese epileptic patients. The therapeutic drug monitoring results of males and females were separately compiled and thereafter each gender group was further divided into children, adults and elderly as different age group. All age groups in both gender groups were evaluated for therapeutic, sub-therapeutic and toxic ranges. It was found that 45% of samples of total samples had sub-therapeutic levels and 55% of all samples had carbamazepine levels in therapeutic range, and none of gender and age group found in toxic range. Compared to males, female samples were more in number of sub-therapeutic levels. Populations of children males and children females were having more samples in sub-therapeutic levels as compared to adult and elderly males and females, respectively. However, it needs further evaluation. The findings of present study revealed that majority of patients were in sub- therapeutic levels. It is suggested that regularly therapeutic drug monitoring of carbamazepine should be performed and dose of carbamazepine in epileptic patients should be adjusted only after therapeutic drug monitoring results in order to assess the compliance, optimize the efficacy, safety and minimize the toxicity.
Keywords
Antiepileptic drugs, carbamazepine plasma levels, TDM
Carbamazepine (CBZ) is a dibenzazepine derivative (carboxamides, Figure 1) used frequently due to its efficiency and economical cost. However, adverse effects of CBZ can be very distressing. CBZ has many dangerous adverse effects, one of which is Stevens- Johnson syndrome (SJS). SJS is an uncommon, life threatening, immune complex hypersensitivity condition involving mucous membrane and skin [1]. CBZ is extensively used in all over the world in the management of epilepsy, trigeminal neuralgia and bipolar disorder [2]. CBZ has several effects on the environment and human. Therefore, assessing the adverse effects of this drug is very essential and valuable [3]. CBZ is nearly entirely metabolized in the body and only slight traces are excreted unchanged in urine. The peak plasma concentration Cmax was 1.9±0.3 μg/ml and the time to reach t1/2 the peak was 19±7 h after a single 200 mg oral extended-release dose of CBZ. The reference range of CBZ concentration has been described to be 4-10 μg/ml. CBZ has complex pharmacokinetics for example auto-induction of metabolism, drug-drug interactions and high serum protein binding that favors use of therapeutic drug monitoring (TDM) [4]. Like other antiepileptic drugs of first generation, central nervous system adverse effects are frequently perceived with higher doses of CBZ. A strong link of dangerous skin reactions with the human leukocyte antigen (HLA) allele HLA-B*1502 has been frequently witnessed in South Asian origin patients, chiefly in Han-Chinese and Indians during CBZ usage [5,6]. Data of these results advocate that Han- Chinese which carries the HLA-B*1502 allele are at higher danger of getting toxic epidermal necrolysis (TEN) and SJS when they use CBZ [6]. Heart defects are the main type of deformities observed in children exposed to CBZ and a high risk of neural tube defects (NTDs) of 0.5-1 % have also been stated on CBZ usage [7]. Findings of one report stated that 6.3 % of infants born to women of South Indian population had cardiac deformities, which were prescribed CBZ as monotherapy [8], other reports have stated that this incidence is only 0.7 % [9]. There are also published data proposing that use of CBZ, could be accountable for fetal malformations but the proof is not yet strong till date [10]. There is also statistically noteworthy proof that CBZ if used as the only anticonvulsant agent causes a doubled risk of fetal deformity [11]. Plasma concentration of CBZ is significantly influenced by many factors; for example age, body weight, gender, auto induction, dose of CBZ and concomitant usage of other drugs [12]. CBZ clearance meaningfully modifies in elderly and as well as children patients and also may be influenced by weight of body [13]. It has been noted generally within a reference range of plasma concentrations, therapeutic effect of most of the antiepileptic drugs accomplished; while too low concentrations are more probably to produce an inadequate effect, and on other hand, too high plasma concentrations are commonly related with serious side effects. TDM is recommended for a number of antiepileptics and usually used as very important tool for individual patients for selecting the optimum therapy regimens. This attitude further apprehends and helps the physicians in knowing why some patients do not respond reasonably to a specific dosage. Additionally, TDM help us to evaluate noncompliance, besides that variation in pharmacokinetics, which arises among and between the individuals and the elements accountable for these type of variation can be examined [14]. Numerous methods are available in literature for the measurement of CBZ in patients of epilepsy including chromatographic and immunoassay methods. High-performance liquid chromatography (HPLC) assays are limited by a lower limit of quantitation, since these assays are not sensitive enough [15]. To overcome these issues, a massspectrometry (MS) is more sensitive and significantly more specific than other liquid chromatography detectors and mass spectrometry provides structural distinctiveness of the distinct components with high molecular specificity and detection sensitivity. The liquid chromatography/mass spectrometry (LC/MS) coupled provides synergistically improved selectivity and sensitivity during separation and detection. Therefore simple, rapid and accurate LC/MS assay method for the quantification of CBZ has been developed, validated and successfully applied in TDM of Chinese epileptic patients in our laboratory. In this study, retrospective analysis of therapeutic monitoring results of CBZ obtained with stated LC/MS method was carried out and besides that, new samples were also quantified with enzyme-multiplied immunoassay technique (EMIT) method, and analysis of TDM results of CBZ obtained with EMIT was also carried out. The rational reason behind choosing an immunoassay method was a good correlation that was found in our laboratory between LC/MS and immunoassay methods for quantification of CBZ in our previous study. The present study is directed towards evaluating and comparing the plasma levels of CBZ in Chinese epileptic patients obtained with above stated assay methods for assessment of compliance, safety and toxicity in different age and gender groups.
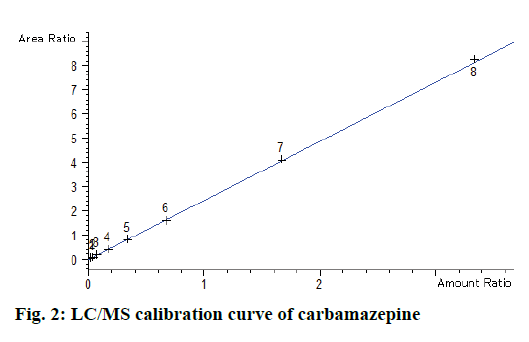
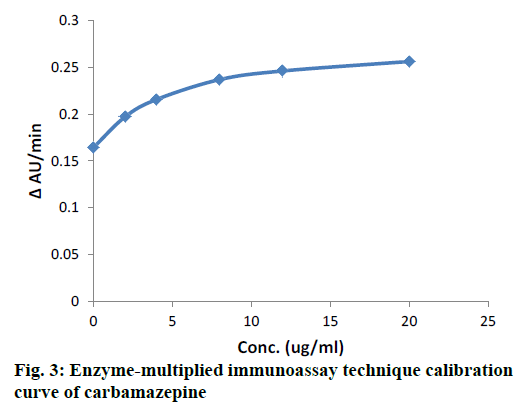
TDM data of CBZ obtained with LC/MS in our laboratory was compiled. Some new samples were also measured with an immunoassay method. CBZ TDM results of total 142 epileptic patients obtained with stated two methods were compiled, evaluated and compared for compliance, safety and toxicity in different age and gender groups of Chinese epileptic patients. The calibration curve of LC/MS is presented in (Figure 2) and calibration curve of EMIT is presented in (Figure 3).
The TDM results of CBZ plasma levels of all patients were compiled in Microsoft Excel system and data was recorded and evaluated by registered pharmacist using statistical software of SPSS. The results were further characterized as per plasma concentrations levels of CBZ into (sub-therapeutic range, therapeutic range and toxic range) and males were separated from females and then each gender group was further subdivided into children, adult and elderly patients as sub-group. The number of male patients (81) was more than female patients (61). All patients were between the ages of 4 to 85 y. The blood samples of epileptic patients who were using CBZ were drawn at Qilu Hospital of Shandong University.
The simple methods for measurement of CBZ has been validated in our laboratory and applied successfully in TDM of CBZ in Chinese epileptic patients. TDM results of CBZ obtained with these methods have been evaluated and compared for assessment of compliance, safety and toxicity in different age and gender groups of Chinese epileptic patients in this study. Chung et al. [16] in a study found a link in carriers of HLA-B*1502 alleles and CBZ-induced SJS/TEN. These all patients were Han-Chinese living in Taiwan during that period, while 101 patients were found as CBZ-tolerant (with no adverse reactions at least 3 mo of expose) and 93 blood samples of randomly selected, biobanked DNA from healthy subjects attended as control subjects. Authors added another new 16 Chinese cases in 2006, with CBZ-induced TEN/SJS and described that out of 60, 59 patients were + for the HLA-B*1502 allele, though the only one patient without HLA-B*1502 was found + for another B15 allele, HLA-B*1558.6. The results of that data suggested that Han-Chinese who carries the HLA-B*1502 allele are at a more higher risk of getting TEN/SJS when they use CBZ, supposing a 0.25 % prevalence of CBZ-induced TEN/SJS in recently recommended CBZ to patients in Taiwan [6]. In our study, 55 % of Chinese patients taking CBZ had drug in therapeutic level and our results were agreed with Kiran et al. [17], they reported that 52.4 % patients had plasma levels of CBZ in therapeutic range, and our findings were little lower to that found by Shakya et al. [18], who reported 79.3 % patients had concentration levels of CBZ in therapeutic levels. The plasma CBZ levels were found in sub therapeutic level in 45 % of patients and none of patients found in toxic levels. The major reason of less plasma concentration of CBZ than predictable may be due to poor patient compliance. Compliance can be improved by restricting to a least the number of daily doses and by monitoring the drug level routinely. The females had 57 % samples in sub-therapeutic levels and males had only 36 % samples in sub-therapeutic levels. Sirmagul et al. [19] reported that combination of phenytoin with CBZ results in higher concentration in men than women. Our potential explanation of these more number of sub-therapeutic samples in females may be due to poor compliance or pregnancy because decreased plasma levels possibly due to increased metabolism of CBZ in pregnancy. As compared to adults and elderly patients in males and females, children males and children females were having more number of samples in sub-therapeutic levels. This may be due to also non-compliance or possibly due to CBZ is more quickly metabolized to their metabolite CBZ- 10, 11 epoxide in young children as compared to adults. The CBZ’s pharmacokinetics in children patients of age 0.3 to 15 y is comparable with that in adults [20]. Demographic information of all patients is presented in (Table 1). The concentration results of CBZ, in males and females are separately presented in (Tables 1 and 2), respectively. CBZ also has diverse physicochemical characteristics, short half-life and narrow therapeutic window. Many medicines could increase the risk of buildup by inhibiting the metabolism. There are some well-known drugs to cause noteworthy rise of CBZ levels i.e. erythromycin and other macrolides. Huge inter-individual variances in apparent plasma halflife are associated with auto-induction and narrow therapeutic window are the main reasons of TDM of CBZ. CBZ plasma levels are straight forward connected with dose, therapeutic effects and adverse effects. Quantifying plasma concentrations are very helpful. A low concentration levels reveals either deprived current compliance or under treatment. Deprived compliance is suspected when recommended dose to patient is not related to measured low concentration or earlier concentration levels guide that the concentration measurement levels should be greater for the certain dose [21]. Several kinds of drugs have interactions with CBZ. In the group of antiepileptics, primidone, phenytoin and phenobarbital increase the clearance of CBZ by two times through induction of CYP3A4, and diminish its half-life, in adults, to an average of 8 h. The CBZ-10–11-epoxide’s clearance also seems to be influenced by enzyme inducers, e.g. it is enlarged around twice by phenobarbital [22]. The present results suggested that there is different metabolic pattern in different gender and age groups. For ensuring maximum efficacy, safety and avoiding toxicity, necessary and routinely therapeutic monitoring should be done in all age and gender groups and dosage should be adjusted on the results of plasma levels of CBZ because clinical response is highly associated with plasma levels of CBZ in epileptic patients.
| Groups | Therapeutic range N (%) |
Sub-therapeutic range N (%) |
Toxic range N (%) |
Total no of samples |
|---|---|---|---|---|
| Children | 7 (44) | 9 (56) | 0 | 16 |
| Adults | 39 (72) | 15 (28) | 0 | 54 |
| Elderly | 6 (54) | 5 (46) | 0 | 11 |
| Total | 52 (64) | 29 (36) | 0 | 81 |
Table 1: Carbamazepine Concentration Levels in Males
| Groups | Therapeutic range N (%) |
Sub-therapeutic range N (%) | Toxic range N (%) |
Total no of samples |
|---|---|---|---|---|
| Children | 5 (36) | 9 (64) | 0 | 14 |
| Adults | 16 (40) | 24 (60) | 0 | 40 |
| Elderly | 5 (71) | 2 (29) | 0 | 7 |
| Total | 26 (43) | 35 (57) | 0 | 61 |
Table 2: Carbamazepine Concentration Levels in Females
In conclusion, The TDM results of CBZ were evaluated and compared for compliance, safety and toxicity in different age and gender groups of Chinese epileptic patients. TDM results showed that almost half of the total samples were in sub-therapeutic levels. The samples of females were more in sub-therapeutic levels as compared to males. The children, male and children female samples were more in sub-therapeutic range as compared to adult and elderly male, and adult and elderly female samples, respectively. The findings of this study are extremely useful and suggesting us that further investigations are required especially in patients with an insufficient seizure control and if patients are taking appropriate dose with proper compliance, than all patients with low concentration levels may require more dosage especially in children due to rapid metabolism of CBZ and this will be especially true when CBZ is co-administered with other antiepileptic drugs. However; it needs further evaluation. Although there is no any sample in toxic range but all patients specially Han-Chinese must be evaluated for HLA-B*1502 alleles prior to CBZ exposure. Since CBZ has low therapeutic range and CBZ is an associated with high risk of serious adverse effects, hence it is suggested that all patients must be screened for HLA-B*1502 alleles prior to prescribing them CBZ and plasma levels of CBZ should be regularly monitored in order to assess the compliance, optimize the safety, efficacy and minimize the toxicity. The present findings are very helpful for neurologists and as well as epileptic patients specially in optimizing the daily dosages of CBZ.
Financial support and sponsorship
This study was supported by Major National Science and Technology Project (2012ZX09303-016-003).
Conflict of interest
The authors declare no conflicts of interest.
References
- Nasir SA, Tan HL, Tan HJ, Hussaini HM, Ramli R. Stevens-Johnson Syndrome following Failure of Genetic Screening prior to Carbamazepine Prescription. Case Rep Dent 2017;2017:4201357.
- Bansal S, Gill M, Bhasin C. Carbamazepine-induced dystonia in an adolescent. Indian J Pharmacol 2016;48(3):329-30.
- Ghafghazi S, MoiniZanjani T, Vosough M, Sabetkasaei M. Interference-free Determination of Carbamazepine in Human Serum Using High Performance Liquid Chromatography: A Comprehensive Research with Three-way Calibration Methods. Iranian J Pharm Res 2017;16(1):120-31.
- Neels HM, Sierens AC, Naelaerts K, Scharpe SL, Hatfield GM, Lambert WE. Therapeutic drug monitoring of old and newer anti-epileptic drugs. ClinChem Lab Med 2004;42(11):1228-55.
- Alfirevic A, Jorgensen AL, Williamson PR, Chadwick DW, Park BK, Pirmohamed M. HLA-B locus in Caucasian patients with carbamazepine hypersensitivity. Pharmacogenomics 2006;7:813-8.
- Hung SI, Chung WH, Jee SH, Chen WC, Chang YT, Lee WR, et al. Genetic susceptibility to carbamazepine-induced cutaneous adverse drug reactions. Pharmacogenet Genomics 2006;16:297-306.
- Kallen AJ. Maternal carbamazepine and infant spina bifida. ReprodToxicol 1994;8(3):203-5.
- Thomas SV, Ajaykumar B, Sindhu K, Francis E, Namboodiri N, Sivasankaran S, et al. Cardiac malformations are increased in infants of mothers with epilepsy. PediatrCardiol 2008;29:604-8.
- Morrow J RA, Guthrie E, Parsons L, Robertson I, Waddell R, et al. Malformation risks of antiepileptic drugs in pregnancy: A prospective study from the UK Epilepsy and Pregnancy Register. Prospective data collected by the UK Epilepsy and Pregnancy Register reports major congenital malformations recorded up to 3 months postnatally. J NeurolNeurosurg Psychiatry 2006;77:193-8.
- Wlodarczyk BJ, Palacios AM, George TM, Finnell RH. Antiepileptic Drugs and Pregnancy Outcomes. Am J Med Genet A 2012;158A:2071-90.
- Vajda FJ, O'Brien TJ, Graham J, Lander CM, Eadie MJ. Is carbamazepine a human teratogen? J ClinNeurosci 2016;23:34-7.
- Chan E, Lee HS, Hue SS. Population pharmacokinetics of carbamazepine in Singapore epileptic patients. Br J Clin Pharmacol 2001;51:567-76.
- Battino D, Croci D, Rossini A, Messina S, Mamoli D, Perucca E. Serum carbamazepine concentrations in elderly patients: a case-matched pharmacokinetic evaluation based on therapeutic drug monitoring data. Epilepsia 2003;44:923-9.
- Patsalos PN, Berry DJ, Bourgeois BF, Cloyd JC, Glauser TA, Johannessen SI, et al. Antiepileptic drugs--best practice guidelines for therapeutic drug monitoring: a position paper by the subcommission on therapeutic drug monitoring, ILAE Commission on Therapeutic Strategies. Epilepsia 2008;49:1239-76.
- Leite CE, Petersen GO, Lunardelli A, Thiesen FV. A high-performance liquid chromatography method for the determination of carbamazepine and carbamazepine-10,11-epoxide and its comparison with chemiluminescent immunoassay. ClinChem Lab Med 2009;47:458-63.
- Chung WH, Hung SI, Hong HS, Hsih MS, Yang LC, Ho HC, et al. Medical genetics: a marker for Stevens-Johnson syndrome. Nature 2004;428:486.
- Kiran D, Piyushal B, Veena SG, Rakesh D, Ghalaut, PS. Therapeutic drug monitoring for antiepileptic drugs using HPLC: An experience at a tertiary care hospital in India. Neurology Asia 2010;15:233-7.
- Shakya G, Malla S, Shakya KN, Shrestha R. Therapeutic drug monitoring of antiepileptic drugs. J Nepal Med Assoc 2008;47:94-7.
- Sirmagul B, Atli O, Ilgin S. The effect of combination therapy on the plasma concentrations of traditional antiepileptics: a retrospective study. Hum ExpToxicol 2012;31:971-80.
- Bertilsson L. Clinical pharmacokinetics of carbamazepine. ClinPharmacokinet 1978;3:128-43.
- Kang JS, Lee MH. Overview of therapeutic drug monitoring. Korean J Intern Med 2009;24:1-10.
- Spina E, Martines C, Fazio A, Trio R, Pisani F, Tomson T. Effect of phenobarbital on the pharmacokinetics of carbamazepine-10,11-epoxide, an active metabolite of carbamazepine. Ther Drug Monit 1991;13(2):109-12.