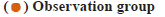- *Corresponding Author:
- Y. L. Huang
Department of Orthopaedics,
Huizhou Central People's Hospital,
Huizhou,
Guangdong 516008,
China
E-mail: kuadan9@yeah.net
| This article was originally published in a special issue, “TrendingTopics in Biomedical Research and Pharmaceutical Sciences” |
| Indian J Pharm Sci 2022:84(1) Spl Issue “131-135” |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
To investigate the efficacy of preemptive analgesia with tramadol injection after single-segment lumbar spinal stenosis surgery is the objective of the study. A total of 120 patients after lumbar spinal stenosis surgery were selected by the random sampling method as the study subjects. Patients were randomly divided into a moderate pain group (control group, n=60) and a preemptive analgesia group (observation group, n=60) according to whether tramadol preemptive analgesia was used. The visual analogue scale score of the two groups were compared at 30 min, 4 h, 8 h, 16 h, 24 h and 48 h after treatment, the number of intramuscular tramadol injections and the total dosage of tramadol administration from the end of surgery to discharge, as well as adverse reactions after treatment. The visual analogue scale score at 30 min, 4 h, 8 h, 16 h and 24 h after surgery of the observation group were significantly lower than the control group (p<0.05). There was no significant difference between the two groups in the visual analogue scale score at 48 h after surgery (p>0.05).The number of intramuscular tramadol injections and the total dosage of tramadol administration from the end of surgery to discharge of the observation group were significantly lower than the control group (p<0.05). The incidence of adverse reactions in the observation group was lower than the control group, but the difference was not statistically significant (p>0.05). Tramadol preemptive analgesia after lumbar spinal stenosis surgery could effectively control pain, reduce the use frequency of postoperative painkillers, reduce the dosage of intramuscular tramadol after surgery and had fewer adverse reactions in the process of treatment to some extent.
Keywords
Lumbar spinal stenosis, tramadol injection, preemptive analgesia, visual analogue scale scores
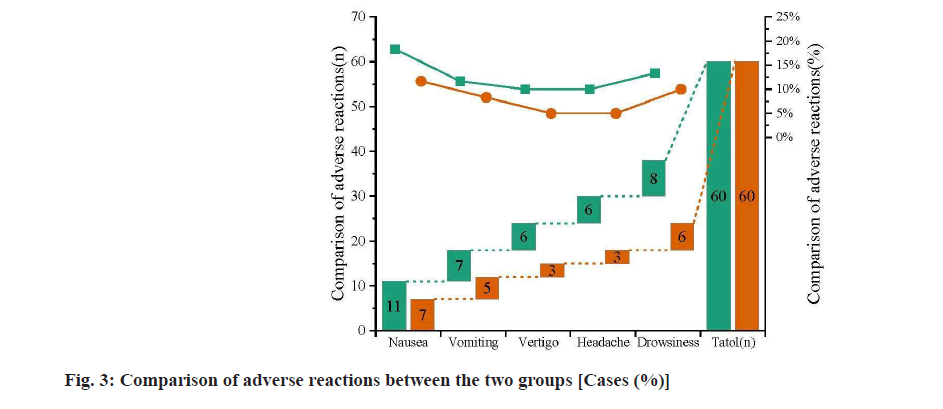
Lumbar spinal stenosis refers to dysfunction due to reduced lumbar canal volume, dural sac and/or nerve root compression, with an incidence of approximately 30 % and a higher incidence in people over 60 y of age [1]. The main symptoms of lumbar spinal stenosis are long-term chronic lower back pain and intermittent claudication [2], which seriously affects the life of patients. Surgery is one of the effective methods to treat lumbar spinal stenosis. Postoperative pain is the most common and most urgent acute traumatic pain in clinical settings [3], manifested as an unpleasant sense in patients feelings and emotions. Spinal surgery is characterized by high pain intensity, severe local inflammatory response and high requirements for postoperative analgesia. Without effective control at the initial stage, continuous pain stimulation can cause pathological remodelling of the central nervous system and hinder the early functional recovery of the spinal joint. Pain has always been a surgery-related concern for surgical patients. A survey of orthopaedic patients cognition and demand for pain nursing in China found that 92 % of patients urgently needed postoperative analgesia, 80 % reported insufficient analgesia and 50 % still had pain after 72 h, indicating a certain gap between patients demand for postoperative analgesia and hospitals analgesia management [4]. Therefore, it is of great clinical significance to strengthen the management of postoperative analgesia after spinal surgery. Preemptive analgesia is a new analgesia method. In recent years, with the rapid development in the physiology, pathophysiology and pharmacology knowledge of pain, preemptive analgesia has started attracting extensive attention [5]. Tramadol hydrochloride is a commonly used analgesic in clinical practice, which is a non-opioid central analgesic. It plays an analgesic role by affecting the transmission of pain sensation and has the advantage of little impact on the respiratory and circulatory systems. However, large doses may cause nausea, vomiting, vertigo and other adverse reactions [6]. This study investigated the analgesic effect and adverse reactions of preemptive analgesia with intramuscular tramadol after single-segment lumbar spinal stenosis surgery, analysed the current postoperative pain problems in patients after lumbar spinal stenosis surgery, with a view to provide a theoretical basis for future pain nursing work after lumbar spine surgery. A total of 120 patients with lumbar spinal stenosis admitted to the department of spinal surgery of our hospital from May 2019 to April 2020 were selected and randomly divided into a moderate pain group (control group, n=60) and a preemptive analgesia group (observation group, n=60) according to the Visual Analogue Scale (VAS) scores for pain. Inclusion criteria includes 30~45 y of age, more than 1 y of disease duration, no response after over 6 mo of conservative treatment; lumbar spinal stenosis confirmed by Computed Tomography (CT) scan or Magnetic Resonance Imaging (MRI) and in line with indications for surgery; for the first time to receive lumbar surgery, no dehydrant/hormone use in the week before surgery; posterior lumbar spinal canal enlarged decompression bone graft fusion; using the same anaesthesia method and the same anaesthetic; signed the informed consent form. Exclusion criteria includes patients complicated with severe cardiopulmonary dysfunction and metabolic diseases; obvious scoliosis and kyphosis in the lumbar spine; multi-segment lumbar spinal stenosis; recently had received or planned to receive surgery on other parts of the body. There was no significant difference in sex distribution, age, lesion segment between the two groups (p>0.05), as shown in Table 1. This experimental scheme has been approved by the medical ethics committee of our hospital. Research medications include tramadol hydrochloride injection (manufacturer: Grunenthal Group, Germany, specification: 100 mg/2 ml). Pain assessment tool include VAS is a 10 cm scale ranging from 0 point at the left end to 10 points at the right end, with 0 point for no pain and 10 points for unbearable pain [7,8]. Injection method is as follows. The intramuscular injection method in basic nursing was adopted. The patient was placed in the supine position. The 1/3 of the top outside the line connecting the anterior superior iliac spine and the coccyx was selected as the injection site and the depth of injection was 2/3. The operating nurses were all qualified nurses who had received the training of preemptive analgesia. Analgesia methods are as follow. The observation group returned to the hospital room after surgery with no complaints of pain. Intramuscular tramadol 100 mg was given when the VAS was 0 point, followed by 100 mg/12 h, continuous administration for 24 h. The control group returned to the hospital room after surgery. Intramuscular tramadol 100 mg was given when the VAS reached moderate pain, followed by 100 mg/12 h, continuous administration for 24 h. After that, for patients in the two groups who still complained of pain and needed analgesic, intramuscular tramadol 100 mg/2 ml was given. Evaluation measures include VAS scores of the two groups at 30 min, 4 h, 8 h, 16 h, 24 h and 48 h after treatment, 0 point for no pain and 10 points for unbearable pain; the number of intramuscular tramadol injections and the total dosage of tramadol administration in the two groups from the end of surgery to discharge; the number of cases developing adverse reactions (nausea, vomiting, vertigo, headache, drowsiness, etc.) in the two groups after tramadol administration. Statistical Package for the Social Sciences (SPSS) 19.0 software was used for statistical analysis. Measurement data were expressed as (x?±s) and the t-test was used for comparison between groups. Count data were expressed in cases (%) and the χ2 test was used for comparison between groups. Statistical significance could be attained when the p-value was less than 0.05. Analgesia effects at different time points after surgery between the groups were compared. The VAS at 30 min, 4 h, 8 h, 16 h and 24 h after surgery of the observation group were significantly lower than the control group (p<0.05). There was no significant difference between the two groups in the VAS at 48 h after surgery (p>0.05) (fig. 1). The number of intramuscular tramadol injections and the total dosage of tramadol administration after surgery between the groups were compared. The number of intramuscular tramadol injections and the total dosage of tramadol from the end of surgery to discharge of the observation group were significantly lower than the control group (p<0.05) (fig. 2). Adverse reactions between the groups were compared. The incidence of adverse reactions in the observation group was lower than the control group, but the difference was not statistically significant (p>0.05) (fig. 3). Pain after orthopaedic surgery is a common postoperative symptom with complicated causes [9]. Pain directly affects patient’s deep breathing and coughing up phlegm and in severe cases may cause atelectasis and pulmonary infection [10]. Severe pain after osteoarticular surgery often makes patients unwilling to engage in limb movement and functional exercise, resulting in insufficient activity, disuse of joint muscle function, joint stiffness and finally the permanent damage of the decline in work and quality of life [11]. Therefore, it is very important to give analgesics in advance and regularly for postoperative analgesia. Effective pain control improves patient’s postoperative physical and psychological comfort, which is the premise of postoperative rehabilitation exercise for patients [12] and conducive to improving patient’s satisfaction with medical work. Therefore, nursing work is crucial for pain relief [13]. Nurses should understand the relevant knowledge of VAS, so as to help patients accurately evaluate postoperative pain and assist doctors to provide timely and effective help for patients with postoperative pain. With the deepening of clinical research, preemptive analgesia and other new methods of analgesia have gradually been applied. Preemptive analgesia is a blocking measure taken before the trauma signals stimulate the body, with the purpose of cutting off the process of peripheral and central nervous sensitization and finally achieving analgesia [14]. Postoperative pain results in abnormal autonomic neural activities and elevated phenolamine in the blood, manifested as tachycardia, elevated blood pressure, arrhythmia, fast breathing, nausea, vomiting, sweating, etc. Meanwhile, the abnormal release of pain-induced and inflammatory mediators not only aggravates the ischemia, hypoxia and oedema of the primary lesion, but also causes abnormal hormone and enzyme metabolism, slower protein synthesis and faster protein decomposition, which is unfavourable to wound healing [15]. The results of this study showed that the VAS in the observation group at 30 min, 4 h, 8 h, 16 h, 24 h and 48 h after surgery were significantly lower than the control group (p<0.05), indicating that the use of preemptive analgesia with tramadol hydrochloride in patients after lumbar spinal stenosis surgery was significant in clinical practice. The number and dosage of postoperative tramadol injections in the observation group were significantly lower than the control group (p<0.05) and the incidence of adverse reactions in the observation group was also lower than in the control group. It suggested that the dosage of tramadol was decreased and the incidence of adverse reactions caused by tramadol was also decreased due to the preemptive analgesia of tramadol. The preemptive analgesia allowed fewer intramuscular injections and lower dosage administration, reducing both the pain of intramuscular injection and the cost of hospitalization and also improving patients satisfaction with analgesia treatment and nursing significantly, which was consistent with the report of Duellman et al.[16] and together reduced the injection workload for clinical nurses. In conclusion, tramadol preemptive analgesia after single-segment lumbar spinal stenosis had significant analgesic effects, in the very great degree reduced the dosage of postoperative tramadol injection and had a lower incidence of adverse reactions in the process of treatment, which to some extent improves the safety of treatment and is worth popularizing and applying in clinical settings.
| Group | Sex (Male/Female) | Age (Year) | Operative segment |
|---|---|---|---|
| Observation group | 42/18 | 38.6±4.2 | L4~L5 in 40 cases, L5~S1 in 20 cases |
| Control group | 42/18 | 38.9±3.0 | L4~L5 in 36 cases, L5~S1 in 24 cases |
Table 1: Comparison of General Materials Between the two Groups (x¯±s, n=60)
Author’s contributions:
Hongbo Wu and Yi Li contributed equally to this work.
Conflict of interests:
The authors declared no conflict of interest.
References
- Kalichman L, Cole R, Kim DH, Li L, Suri P, Guermazi A, et al. Spinal stenosis prevalence and association with symptoms: The Framingham study. Spine J 2009;9(7):545-50.
[Crossref] [Google Scholar] [PubMed]
- Chen J, Wang J, Wang B, Xu H, Lin S, Zhang H. Post-surgical functional recovery, lumbar lordosis, and range of motion associated with MR-detectable redundant nerve roots in lumbar spinal stenosis. Clin Neurol Neurosurg 2016;140:79-84.
[Crossref] [Google Scholar] [PubMed]
- Chinese Academy of orthopedics. Expert advice on the management of common orthopedic pain. Chin J Orthop 2008;28(1):78-81.
- Hu SL, Xu YL, Xiong F. A survey on the cognition and demand of orthopedic inpatients for pain care. J PLA Nurs 2008;25(19):26-7.
- Kelly DJ, Ahmad M, Brull SJ. Preemptive analgesia II: Recent advances and current trends. Can J Anaesth 2001;48(11):1091-101.
[Crossref] [Google Scholar] [PubMed]
- Wang X, Gao SJ, Dong JT, Zheng XZ. Evaluation of the analgesic effect of flurbiprofen axetil combined with tramadol after total knee replacement. Hebei Med J 2014;36(9):1308-10.
- Ferreira-Valente MA, Pais-Ribeiro JL, Jensen MP. Validity of four pain intensity rating scales. Pain 2011;152(10):2399-404.
[Crossref] [Google Scholar] [PubMed]
- Philip BK. Parametric statistics for evaluation of the visual analog scale. Anesth Analg 1990;71(6):710.
[Crossref] [Google Scholar] [PubMed]
- Lai CJ, Li JN. Effect of comprehensive nursing intervention on perioperative pain of patients with pelvic fractures. J Qilu Nurs 2015;2(2):25-6.
- Xiong J, Dong CP, Ouyang LZ. Observation on the effect of intercostal nerve cryosurgery on preventing incision pain after thoracotomy. J Nurs 2006;21(2):26-7.
- Spinal stenosis prevalence and association with symptoms: The Framingham study
- Shang Z. The effect of comfort nursing on the pain of elderly patients with lumbar compression fracture after operation. J Nurs Train 2013;28(2):180-2.
- Debono VB, Zhang S, Ye C, Paul J, Arya A, Hurlburt L, et al. The quality of reporting of RCTs used within a postoperative pain management meta-analysis, using the CONSORT statement. BMC Anesthesiol 2012;12(1):1.
- Li XL, Shen HF, He JX. The application of dexmedetomidine in anesthesia of elderly patients undergoing abdominal surgery. Chin J Clin Ration Drug Use 2015;8(8):72-3.
- Guo XL, Zhou LJ, Zhao JJ. Research progress on the goal of postoperative pain control. J Nurs 2009;16(6):4-6.
- Duellman TJ, Gaffigan C, Milbrandt JC, Allan DG. Multi-modal, pre-emptive analgesia decreases the length of hospital stay following total joint arthroplasty. Orthopedics 2009;32(3):167.
[Google Scholar] [PubMed]
 Control group;
Control group; 
 Contro group;
Contro group;