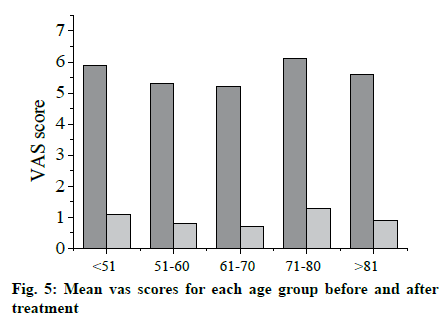- *Corresponding Author:
- Y. Sheng
Department of Dermatology, Huashan Hospital, Fudan University, 12 Middle Wulumuqi Road, Shanghai 200040, China
E-mail: shengyouyu_felix@126.com
| This article was originally published in Special issue on “Trends in therapeutic Management of Various Conditions” |
| Indian J Pharm Sci 2020:82(3) spl issue 6;105-111 |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
In order to evaluate the pain of patients with herpes zoster and to study the analgesic treatment, 100 patients with herpes zoster are enrolled in this study. Patients with herpes zoster are classified and admitted to the hospital using oral descriptive scoring. The pain is assessed on a graded basis, and the visual analog scale is used to assess the pain before and after treatment. It is found that patients with herpes zoster are mainly middle-aged and elderly, and the course of disease is usually 2-3 w. After age grouping studies, there is no significant difference in pain levels between different age groups, and the VRS scores at admission are basically 3-4, showing that the pain caused by herpes zoster is very intense. After treatment, the VAS scores of patients before and after treatment are statistically found to greatly improve the pain of the patients, and to avoid the patient’ s normal life due to pain.
Keywords
Herpes zoster, pain assessment, visual analogue scale, verbal rating scales
Herpes zoster (HZ) is a viral skin disease characterized by herpes zoster and neuralgia caused by varicellazoster virus (VZV) invading the ganglia and skin, causing the virus to distribute along the peripheral nerves[1,2]. The rash occurs on one side of the body and is distributed along the ganglion inner area. Generally, it does not exceed the median line, and the skin between the groups is normal[3]. Severe patients and immunocompromised patients are often accompanied by multiple lesion areas. Herpes zoster is a viral skin disease caused by varicella-zoster virus (doublestranded DNA virus) infection, which is more common in the clinic and occurs in adults[4]. After the original infection of chickenpox, the virus can persist in the posterior root ganglia of the spinal cord, and the disease occurs when the body’ s immune function is low (such as cold, overwork, infection, tumor, radiotherapy and chemotherapy). Under the influence of various predisposing factors, the virus is stimulated, causing inflammation and necrosis of the invaded ganglia, causing neuralgia, and the reactivated virus can move along the peripheral nerve fibers to the skin to produce skin lesions[5]. Herpes zoster is a common clinical skin disease that can occur at any age and is more common in adults and the elderly. Clinical manifestations are mostly skin lesions and severe neuralgia. With the accelerated pace of modern life, increased pressure in all areas, and the aging of the world population, the incidence of herpes zoster has gradually increased[6]. Herpes zoster often occurs in spring and autumn. Before the onset, there are often prodromal symptoms such as low fever, fatigue, general discomfort, and loss of appetite. Skin-affected areas generally have a burning sensation, neuralgia or anthill sensation, itching, and herpes. However, there are also those who have no prodromal symptoms[7]. The initial skin lesions are red papules and maculopapular rashes. After about 3~4 d, the miliary size of the clusters of miliary herpes is formed, and the blister is formed rapidly. The blister wall is intense and the lesions can be transformed into hemorrhagic, necrotic or bullous damage. It is arranged in a strip along the direction of the nerve, and generally it does not exceed the trunk midline. Local lymph nodes often have swelling and pain[8]. The rash occurs mostly in the sensory nerve and cranial nerve distribution area of the spinal cord. It is most common in the cranial nerve to be affected by the distribution of the trigeminal nerve. After 3 to 4 d of rash, the blister fluid changes from transparent to turbid, then dry and crusted, leaving no scar after removal. The lesion is very sensitive to any stimuli, and a slight touch can cause severe pain. Some patients still have neuralgia after the lesion has completely subsided, and this post-herpetic neuralgia can last for several months. The overall course of children and young people are generally 2 to 3 w, and the elderly are about 3 to 4 w. The incidence of herpes zoster is mostly related to the infection, excessive fatigue, mental stress, trauma, tumors, systemic diseases and other incentives that cause the body’s immunity to decrease[9]. In this study, 100 patients with herpes zoster who are eligible for dermatology hospitalization in Huashan Hospital, Fudan University from September 2013 to September 2018 are studied. The diagnostic criteria are in accordance with Chinese Clinical Dermatology (2nd Edn). The following typical clinical symptoms and signs: along the unilateral nerve, irregular erythema, clustered papules, herpes, or small blisters appear in the area, arranged in a strip shape. The rash generally does not exceed the midline of the body, often accompanied by neuralgia or skin paresthesia. The informed consent signed by the patients or their family members was obtained and this study was approved by the medical ethics committee of Huashan Hospital, Fudan University. The inclusion criteria: People meet the criteria for the diagnosis of herpes zoster in Chinese clinical dermatology. People are older than 14 y of old. The main medical record data required is complete and people can be interviewed after 1 mo of discharge. Exclusion criteria: People who do not meet the criteria for inclusion in the medical record. People are not fully treated, who are discharged automatically. People have been transferred to other diseases. General clinical classification: According to the shape, area, blister content of the skin lesions, herpes zoster can be divided into 7 categories. Vulgaris: On the basis of erythema, clustered miliary to soy-sized herpes, and blisters can be seen. The blister fluid is clear. The rash is distributed on one side, which generally does not exceed the midline, accompanied by neuralgia or skin paresthesia. This type is most common in the clinic. Incomplete type: It is also known as the frustration type. There is only neuralgia without skin lesions, or only erythema and papules without typical blisters. Bullous type: During the onset of the disease, large blisters above the size of broad beans will appear. Hemorrhagic type: The blister contents are bloody. Gangrene type: The center of the skin lesions will be necrotic, ulcerated, and crusted. The crusted skin is not easy to fall off and scars will be left after healing. Dissemination type: It is also known as pan-hair type, involving 2 or more ganglia to produce lesions on the contralateral or ipsilateral multiple areas. This type occurs mostly in immunosuppressive patients with underlying diseases, so it is more common in patients with frail or malignant lymphoma. A few days after the local skin lesions appear in the patient, there is a similar varicella-like rash, which may be accompanied by high-heat, fatigue and other systemic symptoms, which may be complicated by lung and brain damage. If the patient is seriously ill, death may occur. Nodular type: In combination with HIV-infected individuals, some skin lesions can develop into nodular lesions with scars.
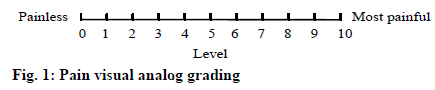
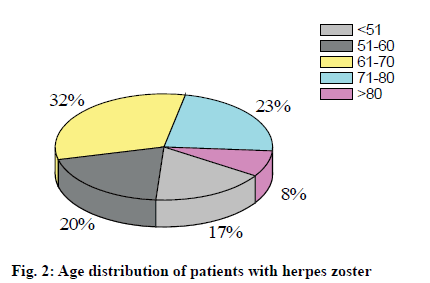
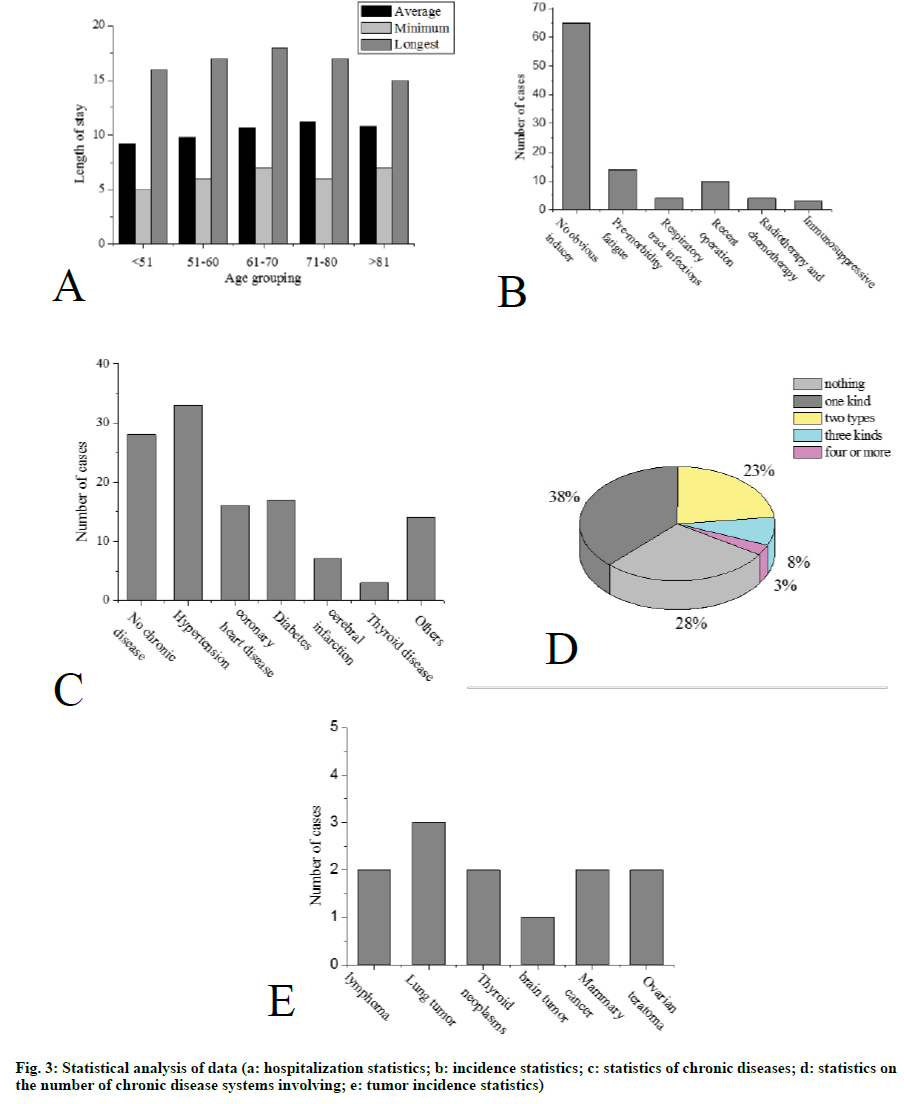
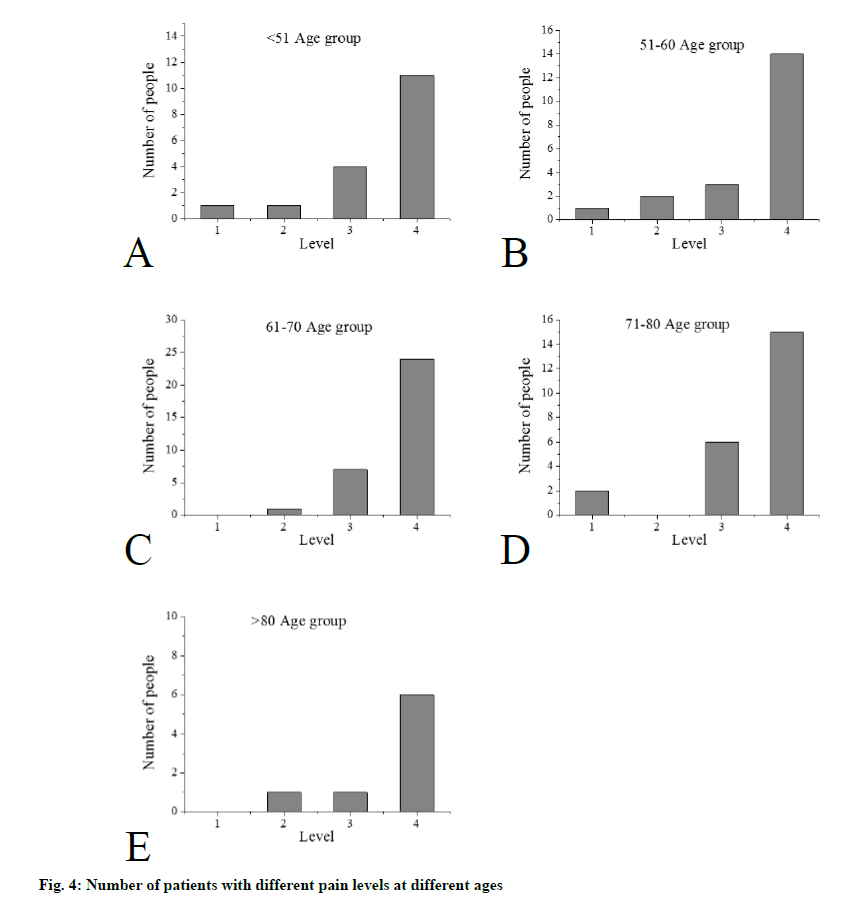
According to the lesion site and the affected nerve, it can be divided into five types. Trigeminal nerve zoster: The trigeminal nerve is divided into the ocular branch, the maxillary branch and the mandibular branch. Eye herpes zoster: It is the involvement of the eye, involving the cornea and conjunctiva. The clinical manifestations are redness and swelling of the face, conjunctival congestion, periocular blisters, ulcers, and crusting. Ulcerative keratitis can form after blistering of the cornea, and scar formation can lead to blindness. In severe cases, total ocular inflammation, encephalitis, acute retinal necrosis syndrome, and even death will occur. When the virus invades the nasal branch of the eye, there is often a blister on the tip of the nose, which is the Hutchinson sign. Maxillary herpes zoster: Blisters often appear in the upper mucous membrane, palate, and tonsils. Mandibular herpes zoster: Blisters appear in the front of the tongue, at the bottom of the mouth, and in the buccal mucosa. Usually, toothache is the first symptom of trigeminal herpes zoster. Herpes zoster oticus: It is caused by the virus invading the auditory nerve and facial nerve, causing local inflammatory edema and compression of nerves. Symptoms include herpes in the external auditory canal or tympanic membrane, and hearing and other symptoms such as tinnitus and deafness. There will also be symptoms such as loss of taste in the front 2/3 of the tongue, tearing, blisters in the nose, dizziness, nausea, vomiting and nystagmus. Ramsay-Hunt syndrome: It is the involvement of the geniculate ganglia, which affects the movement of the facial nerve and the sensory fibers. It produces facial tribes, earaches and triads of the external ear canal. Herpes-type facial paralysis (ZSH): It is also known as atypical herpes facial paralysis. It is often accompanied by ear, pharynx and head and neck pain, dizziness, hearing loss and other symptoms, but not accompanied by the appearance of typical ear herpes. Zoster meningoencephalitis: The virus invades into the central nervous system or metamorphosis along the nerve fibers of the anterior and posterior roots of the spinal cord. There are headaches, vomiting, convulsions or other progressive sensory disturbances, as well as ataxia and other cerebellar symptoms. Motor paralysis: It is caused by motor nerve involvement, and the performance varies depending on the involved nerves. In the lower thoracic nerve, if the 10th and 11th motor nerve roots are involved, abdominal wall spasm may occur. Invasion of the perianal genital nerve may cause defecation and dysuria. Although the symptoms of paralysis last longer, from w to months, most can be recovered. Visceral zoster: The virus invades the splanchnic nerve fibers of the sympathetic and parasympathetic nerves from the posterior root ganglia of the spinal cord. When the digestive system nerve is involved, segmental gastroenteritis will occur. When the urinary nervous system is involved, unilateral bladder mucosal ulcers occur. When the peritoneum and pleura are involved, irritation may occur in the corresponding site, and severe fluid may have symptoms such as effusion. Visual analogue scale/score (VAS) and a more concise Verbal rating scales (VRS) are used in this study. Visual analogue score method: The most painful point within 24 h before the observation point is recorded. It means that, with a 10cm VAS scale, a straight line is divided into 10 parts. The initial is 0, which means no pain, and the end is 10, which means unbearable severe pain. The middle indicates different levels of pain. Among them, 1-3 is mild, 4-6 is moderate, and 7-10 is severe. The patients mark the location that best represents the pain, as shown in figure 1, and the observer records the reading. A 4-level scoring method is used in the oral descriptive scoring method. Level 1: It is completely painless. Level 2: It is mild pain. Patient is tolerable. Daily life and sleep are not disturbed. Level 3: It is moderate pain. The patient’ s pain is obviously not tolerance. Daily life is not disturbed, but it will affect sleep, which requires taking analgesic drugs. Level 4: It is severe pain. Patients with severe pain cannot tolerate. Daily life and sleep are severely interfered. It may be accompanied by a passive position or autonomic disorder, and an analgesic drug must be used. The degree of pain is judged and recorded by the case collector based on the description of the patient’ s pain condition in the hospital history record. Treatment: Each time 300mg of valacyclovir hydrochloride (Livzon Group Livzon Pharmaceutical Factory China) is taken orally twice a day. Each time 10mg of vitamin B1 is taken orally three times a day. Local skin treatment of rash: The skin lesions were applied wet with saline. According to the degree of herpes regression and pain relief, the effect is evaluated. Healing: The skin lesion completely subsides, and the pain completely disappears. Markedly: The skin lesion subsides ≥75%, and the pain basically disappears, occasionally stinging. Improved: 50% ≤ skin lesions subside < 75%. The pain has been alleviated. Ineffective: Skin lesions subsides <50%. There is no significant reduction in pain. The statistical software uses spss23.0, SAS, and the measurement data are expressed by the mean standard deviation (X±s). The comparison between the mean of the different groups is analyzed by ANOVA. The comparison between the data of the counting data is performed by chi-square test or the exact probability method Fisher. The rank data rate comparison is performed by rank sum test, the correlation analysis is performed by Spearman rank correlation coefficient, and the chi-square test is used in the same data set to compare the significant level with Bonferroni method before the pairwise comparison. The influencing factors are analyzed by logistic regression analysis. The difference is statistically significant at p<0.05. A total of 100 subjects are included in the study, including 48 males (48%) and 52 females (52%). The average age of onset is 53.5 y old, the minimum age is 31 y old, and the maximum age is 87 y old. Among them, patients aged < 51 y old, are 17 cases, 20 cases of 51-60 y old, 32 cases of 61-70 y old, 23 cases of 71-80 y old, and 8 cases of > 81 y old, as shown in fig. 1. The average hospital stay in 100 patients is about 11 d, the longest hospital stay is 18 d, and the shortest hospital stay is 5 d. The statistics of hospitalization days for each age group are shown in fig. 3A. The cause of the patient’ s morbidity is shown in fig. 3B. The number of patients with chronic diseases is shown in fig 3C. According to cardiovascular diseases, respiratory diseases, digestive diseases, urinary system diseases, endocrine diseases, nervous system diseases, blood system diseases, reproductive system diseases, sports system diseases, mental system diseases, rheumatism and immune diseases, infectious diseases classification of skin diseases, statistics on the number of patients with chronic disease systems are shown in fig. 3D. The patient’ s tumor incidence statistics are shown in fig. 3E. According to the VRS classification, the number of patients with different pain levels at different ages in admission to 100 subjects is shown in fig. 4. Kruskal- Wallis test is used to compare the pain degree of each age group. The results show that there is no significant difference between different age groups and pain grade (H=5.257, P>0.05). In the 50-year-old group, the subjects are divided into <51-year-old group and ≥51-year-old. The difference between the two groups is compared between the two groups by the rank-sum test. The results show that the degree of pain is grade 4. There are no significant differences between the two age groups in the patients (Z=-0 A: the number of patients with different pain levels in <51 y old; B: the number of patients with different pain levels in 51-60 y; C: the number of patients with different pain levels in 61-70 years old; D: the number of patients with different pain levels in 71-80 y old; E: the number of patients with different pain levels in >81 years old) According to age grouping, VAS scores are performed on each group of patients. The average VAS scores of each group before and after treatment are shown in fig. 5. Among the 100 patients with herpes zoster virus rash studied in this study, there are slightly more women than men, which is basically consistent with most of the results in recent years, but it is not completely certain that the incidence of herpes zoster must be greater than that of men, and more needs to be done. Follow-up studies of large sample sizes and more regions are clear. The results of this study show that patients with herpes zoster are mainly middle-aged and elderly, and the peak age of onset is 60-69 y old. About 83% of hospitalized patients are older than 50 y old, and about 63% of patients are older than 60 y old. The course of herpes zoster is usually 2-3 w, and the elderly are slightly longer, about 3-4 w. After the antiviral treatment is enough, it is decided whether to discharge according to the outcome. At the same time, the hospital stay is also affected by the actual situation such as the cost, medical insurance restriction, and the willingness of the patients and their families. The maximum length of hospital stay in this study is 18 days, and the shortest is 5 days. According to the VRS-4 classification method, the pain is divided into four pain levels. From the statistical results, it can be seen that the pain level of 100 subjects at the time of admission is mostly distributed at grades 3 and 4. At the same time, it can be seen from the analysis results that there is no significant difference in the degree of pain in different age groups, which shows that the pain caused by herpes zoster is very large. After treatment, the VAS scores of patients before and after treatment are statistically found to significantly improve the pain of the patients and significantly reduce the VAS score.
References
- Dayan RR, Peleg R. Herpes zoster – typical and atypical presentations. Postgraduate Medicine, 2017; 129(6): 567.
- Cheng X, Zhao SL, Zhang HM. AF1q gene polymorphism proteomic markers in herpes zoster-infected leukemia patients. J Biol Regul Homeost Agents, 2019; 33(2): 505-10.
- Varghese L, Standaert B, Olivieri A. The temporal impact of aging on the burden of herpes zoster. Bmc Geriatrics, 2017; 17(1): 30.
- Yang SY, Li HX, Yi XH. Risk of Stroke in Patients with Herpes Zoster: A Systematic Review and Meta-Analysis. J. Stroke Cerebrovasc Dis 2017; 26(2): 01.
- Alicino C, Trucchi C, Paganino C. Incidence of herpes zoster and post-herpetic neuralgia in Italy: Results from a 3-years population-based study. Hum Vaccin Immunother 2017; 13(2): 399-404.
- Kim K. Pulsed Radiofrequency to the Dorsal Root Ganglion in Acute Herpes Zoster and Postherpetic Neuralgia. Pain Physician 2017; 20(3): E411.
- Sato K, Adachi K, Nakamura H. Burden of herpes zoster and postherpetic neuralgia in Japanese adults 60 years of age or older: Results from an observational, prospective, physician practice‐based cohort study. J Dermatol 2017; 44(4): 414-22.
- Friesen KJ, Dan C, Falk J. Cost of shingles: population-based burden of disease analysis of herpes zoster and postherpetic neuralgia. Bmc Infect Dise 2017; 17(1): 69.
- Kim JY, Park GH, Min JK. Usefulness of Inflammatory Markers for the Prediction of Postherpetic Neuralgia in Patients with Acute Herpes Zoster. Annals Dermatol 2018; 30(2): 158-63.