- *Corresponding Author:
- Li Xu
Department of Neurosurgery, Pukou Branch Hospital of Jiangsu Province Hospital (Nanjing Pukou Central Hospital), Nanjing, Jiangsu 211800, China
E-mail: xl13675155987@sina.com
| This article was originally published in a special issue, “New Advancements in Biomedical and Pharmaceutical Sciences” |
| Indian J Pharm Sci 2022:84(2)Spl Issue “1-7” |
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms
Abstract
To study the value of cranial ultrasound in premature infants. A total of 150 newborns were selected for cranial ultrasound examination within 48 h of birth. According to the classification criteria, they were diagnosed as intraventricular hemorrhage in premature infants and punctate white matter damage. The children were graded and compared with the magnetic resonance imaging results to analyze the brain development maturity and the characteristics of brain injury in this kind of premature infants. At the same time, the gray value of the abnormal white matter area was measured and the gestational age was corrected and followed up for 1 y. The Bayley Scales of Infant Development was used to evaluate the psychomotor development index, mental developmental index; Pearson analysis method analyzes the relationship between the gray value of brain ultrasound, psychomotor development index and mental development index. Cranial ultrasound examination revealed 49 cases of pure intraventricular hemorrhage in premature infants, 41 cases of intraventricular hemorrhage in premature infants combined with ventricular enlargement, 10 cases of intraventricular hemorrhage in premature infants combined with punctate white matter damage, 2 cases of simple punctate white matter damage, 46 cases with no obvious abnormalities. After 1 y follow-up, 102 cases of normal preterm infants and 46 cases were abnormal; intraventricular hemorrhage in premature infants, punctate white matter damage 6 cases of premature infants assessed as grade IV, motor and mental retardation rate was 100 % (6/6); 10 cases of preterm infants assessed as grade III by intraventricular hemorrhage in premature infants, motor retardation rate 70 % (7/10), mental retardation rate of 90 % (9/10), 8 cases of premature infants evaluated by punctate white matter damage as grade III, motor developmental retardation rate of 50 % (4/8), mental retardation rate of 62.5 % (5/8), intraventricular hemorrhage in premature infants, punctate white matter damage degree and premature delivery. There was a statistically significant difference in children’s motor and mental retardation (p<0.05); the gray value of the brain ultrasound after the birth of premature infants was negatively correlated with psychomotor development index and mental development index (r=-0.830, p<0.05; r=-0.917, p<0.05). The higher the evaluation levels of intraventricular hemorrhage in premature infants and punctate white matter damage, the higher the gray value and the worse the neonatal movement and intellectual development.
Keywords
Cranial ultrasound, premature infants, intraventricular hemorrhage, brain white matter damage, motor development, intellectal development
The subependymal tissue of preterm infants with very low body weight has abundant capillaries and relatively loose structure, which leads to the lack of connective tissue support. Therefore, acidosis is prone to occur, leading to hypoxia disintegration, necrosis, bleeding and so on. When the amount of bleeding is large, the ependymal rupture causes blood to enter the lateral ventricle and eventually causes sudden death in the child [1]. With the improvement of medical technology, the survival rate of ultra-low and very low birth weight infants has increased significantly. However, the incidence of White Matter Damage (WMD) is gradually increasing, which is a common form of brain damage in clinical premature infants. It is reported that the incidence of white matter injury in preterm infants in China is as high as 30 % and most of the surviving preterm infants are associated with longterm neurodevelopmental abnormalities [2]. Among the extremely premature infants <30 w of gestational age, 10 %~15 % developed cerebral palsy, 40 %~50 % showed mild motor dysfunction and more than 50 % had long-term cognitive learning dysfunction, which are related to abnormal brain development caused by WMD [3]. However, having no clinical manifestations, nearly 50 % of premature infants must rely on imaging examination. Cranial ultrasound has the advantages of low cost, low damage, convenient and quick, which is of great significance for the early diagnosis of brain injury in preterm infants and has become a practical and reliable method for the diagnosis of periventricular leukinomalacia and intracranial hemorrhage in preterm infants [4,5]. In this study, cranial ultrasound was used to examine the conditions of brain injury in premature infants and the gray value of WMD region was measured, so as to evaluate the motor and intellectual development of premature infants and to find the relationship between prognostic indicators and imaging measurements, so as to provide reference for the longterm prognosis of craniocerebral injury in premature infants. The report is as follows.
Materials and Methods
Subjects:
A total of 150 neonates with gestational age of 30 to 40 w admitted to the Department of Neurosurgery, Nanjing Pukou central Hospital from January 2019 to May 2020 were selected. One died during hospitalization and another could not be followed up, leaving 148 patients for study. In inclusion criteria, 26 to 36 w gestational age, (32.20±1.15) w average gestational age, 805 to 2990 g birth weight, (2133.10±525.10) g average birth weight, 89 cases of vaginal delivery, 59 cases of cesarean section, all of the children received regular treatment, artificial feeding was the main method and their families had signed informed consent. Exclusion criteria include congenital malformation and abnormal brain development, chromosomal abnormalities and metabolic diseases, central nervous system infection, cerebellar hemorrhage. There were 79 males and 69 females. The diagnosis of white matter injury in premature infants was in line with the diagnostic criteria of brain injury in premature infants established by the Neonatal Professional Committee of the Chinese Medical Doctor Association.
Instrument:
The Siemens ultrasonic diagnostic system (Acuson X700) produced by Siemens AG of Germany was adopted and 4~10 MHz phased array probe combined with 5~14 MHz linear array probe were selected.
Methods:
The coronal plane, transverse plane and sagittal plane of the brain were scanned with a fan-shaped probe. The linear array probe was used to scan the superficial brain tissue and subarachnoid space. Main observed in children with brain ditch, lobes and gyri parts development situation, development situation, the cerebellum subdural and subarachnoid hemorrhage, fluid, brain tissue echo is abnormal limitations or diffuse, an abnormal presence of ventricular morphology or ventricle enlarge, interior echoes choroid plexus and brain morphology is normal, etc. All children were examined by craniocerebral ultrasound examination within 48 h of birth and further Magnetic Resonance Imaging (MRI) examination was performed if brain injury was found. Cerebral ultrasound was monitored once a day in the progressive stage and once every 3 to 7 d in the stable stage until the child were discharged from hospital.
Intraventricular Hemorrhage in Premature Infants (PIVH) diagnostic criteria:
Intraventricular-strong, increased or lumpiness of echo around the ventricle, epidural or subdural space, subarachnoid space. The intraventricular and periventricular hemorrhage was divided into four grades based on the Papile grading method [6], grade I-pure subependymal hemorrhage, confined to the caudate nucleus head area of the anterior horn of the lateral ventricle, and ultrasonographic manifestations were lump-like hyperecho under the anterior horn of the lateral ventricle; grade II-subependymal hemorrhage into the ventricle, causing intraventricular hemorrhage. Ultrasonographic findings showed massive or patchy hyperechoic masses beside the choroid plexus in the ventricle without ventricular dilation; grade IIIhemorrhage with ventricular dilation, ultrasound showed lumpiness hyperecho with ventricular dilation and grade IV, intraventricular hemorrhage with ventricular dilation and spread to other parts of the brain.
Ultrasonography showed spherical hyperecho above the ventricle. The Papile grading of intraventricularperiventricular hemorrhage is shown in fig. 1.
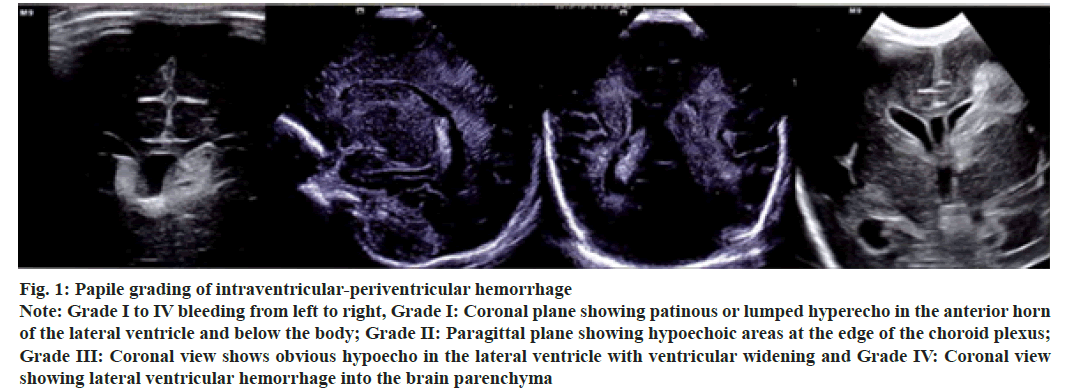
Figure 1: Papile grading of intraventricular-periventricular hemorrhage
Note: Grade I to IV bleeding from left to right, Grade I: Coronal plane showing patinous or lumped hyperecho in the anterior horn of the lateral ventricle and below the body; Grade II: Paragittal plane showing hypoechoic areas at the edge of the choroid plexus; Grade III: Coronal view shows obvious hypoecho in the lateral ventricle with ventricular widening and Grade IV: Coronal view showing lateral ventricular hemorrhage into the brain parenchyma
Criteria for ventricular dilatation:
The normal shape of the anterior horn of the lateral ventricle is horn-like or slit-like. When widened, the forefoot appears slightly rounded shape first and the degree of rounded shape gradually increases and the natural bending radian gradually disappears and finally forms a ball. Mild 4~6 mm, moderate 6~10 mm and severe more than 10 mm. The normal shape of the ventricle is slit, with a width of about 2~3 mm, suggesting an enlarged standard width of Blood-Brain Barrier (BBB) 0.3 mm and gradually elliptical or circular shape.
Punctate White Matter Damage (PWMD) classification criteria:
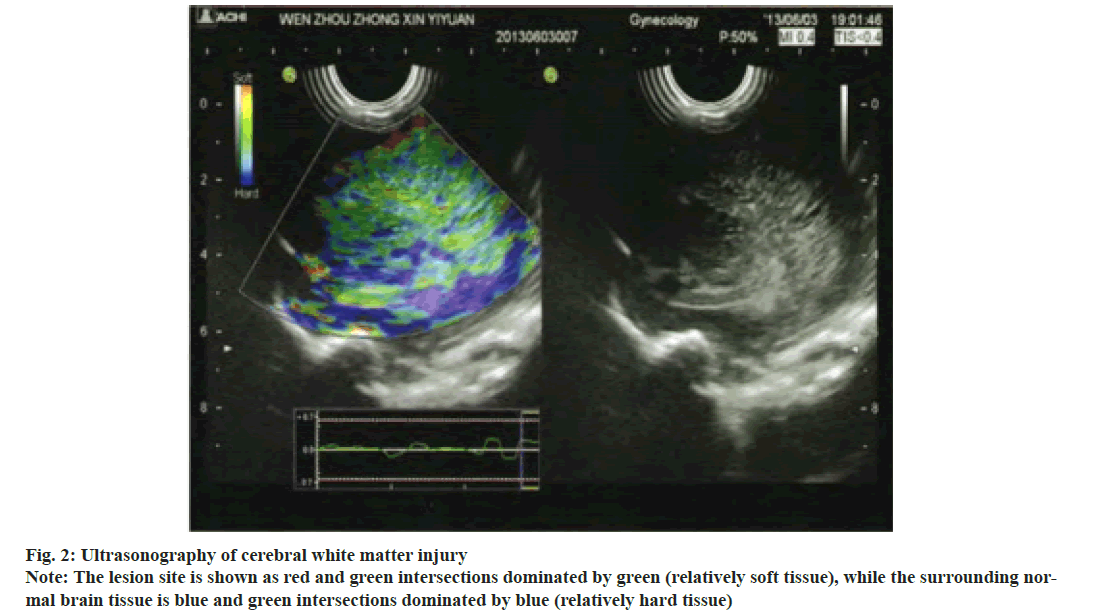
Grade I, transient enhancement of periventricular white matter echo; grade II, enhanced periventricular white matter echo with or without focal small cysts; grade III, the periventricular white matter echo was significantly enhanced with or without multifocal cystic changes and grade IV, diffuse white matter echoes around the ventricle are significantly enhanced with or without multifocal cysts. The ultrasonography of white matter injury in the same part of the brain in the same child as shown in fig. 2.
Measurement of cranial ultrasonic gray value:
The 1 cm2 area of abnormal white matter was selected. The average gray value in the selected area was measured by image analysis software. Extremely strong echo areas were excluded in the calculation.
Assessment of motor and intellectual development of preterm infants after correction of month age:
148 cases of preterm infants were corrected for 12 mo according to the expected date of birth and the motor and intellectual development of the infants was assessed by Bayley’s Infant Development Scale [7]. According to the scoring method, the scores were converted into equivalent Psychomotor Development Index (PDI) and Mental Development Index (MDI) to divide the developmental grades. Both scores ranged from 0 to 114, mild developmental delay was 70 to 84 and developmental delay was <69. A score of >85 indicated normal development, while a score of <85 indicated abnormal development.
Statistical treatment:
All data in this study were processed by Statistical Package for the Social Sciences (SPSS) 22.0 software package. Counting data is expressed as Percentage (%). Chi-square test or Kruskal Wallis H test were used for comparison between groups. The measured data were expressed as mean±standard deviation. Analysis of variance was used for comparison between groups. Correlation analysis was performed using Pearson analysis. The test level was p<0.05, indicating statistically significant difference.
Results and Discussion
The results showed that 49 patients (33.11 %) had simple PIVHs, including intraventricular-periventricular hemorrhage, extradural hemorrhage, subarachnoid hemorrhage and subdural hemorrhage. PIVH was complicated with ventricular enlargement in 41 cases (27.70 %), including mild enlargement in 13 cases (31.71 %), moderate enlargement in 19 cases (46.34 %) and severe enlargement in 9 cases (21.95 %). After clinical treatment, 31 cases returned to normal. PIVH combined with PWMD in 10 cases (6.76 %). Simple PWMD2 cases (1.35 %). No obvious abnormality was found in 46 cases (31.10 %). The preterm infants were followed up for 12 mo after correction. There were 26 children with PIVH and PWMD. There were 7 cases of PIVH I+PWMD I, 4 cases of PIVH I+PWMD III, 2 cases of PIVH II+PWMD III, 4 cases of PIVH IIII+PWMD III, 4 cases of PIVH III+PWMD III and 5 cases of PIVH IV+PWMD IV. According to PDI and MDI scores, 102 cases (68.92 %) were normal premature infants and 46 cases (31.08 %) were abnormal premature infants. According to PIVH classification, 74 cases (50.00 %) were normal preterm infants, including 32 cases (21.62 %) in grade I, 26 cases (17.57 %) in grade II, 10 cases (6.76 %) in grade III and 6 cases (4.05 %) in grade IV. According to PIVH classification, 78 cases of normal premature infants (52.70 %), 26 cases of grade I (17.57 %), 30 cases of grade II (20.27 %), 8 cases of grade III (5.41 %) and 6 cases of grade IV (4.05 %) were shown in Table 1.
6 cases of preterm infants rated as grade IV by PIVH and PWMD. Among them, 2 patients with a diameter of 25 mm were accompanied by compression deformation of the lateral ventricles on the affected side, deviation of the cerebral line and dilation of the contralateral lateral ventricles. During follow-up observation, 2 parents chose to give up treatment. Among the other 4 surviving preemies, 3 had pseudocyst which was not the same as the lateral ventricle and 1 had perforation deformity which was the same as the lateral ventricle. There were 10 preterm infants with PIVH and 8 preterm infants with PWMD.
6 cases of preterm infants rated as grade IV by PIVH and PWMD. The rate of motor and mental retardation was 100 % (6/6). 10 cases of preterm infants rated as grade III by PIVH. The motor development retardation rate was 70 % (7/10). Intellectual retardation rate was 90 % (9/10). 8 cases of preterm infants rated as grade III with PWMD. The motor development retardation rate was 50 % (4/8). The rate of mental retardation was 62.5 % (5/8). There were significant differences in the degree of PIVH, PWMD and motor and mental retardation of premature infants (PIVH: H=80.503, p<0.05; PWMD: H=91.524, p<0.05), as shown in Table 1.
| Project | PDI | MDI | |||
|---|---|---|---|---|---|
| Normal (n=102) | Abnormal (n=46) | Normal (n=102) | Abnormal (n=46) | ||
| PIVH | Normal | 49 | 25 | 55 | 19 |
| I | 29 | 3 | 27 | 5 | |
| II | 21 | 5 | 19 | 7 | |
| III | 3 | 7 | 1 | 9 | |
| IV | 0 | 6 | 0 | 6 | |
| PWMD | Normal | 59 | 19 | 57 | 21 |
| I | 21 | 5 | 21 | 5 | |
| II | 18 | 12 | 21 | 9 | |
| III | 4 | 4 | 3 | 5 | |
| IV | 0 | 6 | 0 | 6 | |
Table 1: Ultrasound Examination of PDI AND MDI in Normal and Abnormal Children (Cases)
The ultrasonographic grayscale scores of PDI and MDI were (94.30±2.14) points and (93.15±3.05) points respectively in normal preterm infants 12 mo after correction. The ultrasonographic grayscale scores of abnormal premature infants were (122.59±3.90) and (124.91±4.30), respectively. The results showed that there were statistical differences in ultrasonic gray values of preterm infants with different prognosis (t=- 46.164, 45.226; p<0.01). In order to verify the significant influence between PDI, MDI and ultrasonic gray value, homogeneity of variance test was first conducted on the variables and the results are shown in Table 2. The significance results of homogeneity of variance test were 0.132 and 0.128, indicating homogeneity of sample variance.
| Variable | Levene | df1 | df2 | p |
|---|---|---|---|---|
| PDI | 1.902 | 2 | 145 | 0.132 |
| MDI | 1.897 | 2 | 145 | 0.128 |
Table 2: Homogeneity Test of Variances
Table 3 shows the results of one-way Analysis of Variance (ANOVA). F value is 28.450 and 5.940, respectively and p value is 0.000, less than 0.05, indicating that PDI, MDI and ultrasonic gray value are significantly correlated.
| Variable | Sum of squares | df | Mean square | F | p | |
|---|---|---|---|---|---|---|
| PDI | Between groups | 386.146 | 2 | 520.50 | 28.450 | 0.000 |
| Within the group | 314.424 | 145 | 65.205 | |||
| total | 700.57 | 147 | ||||
| MDI | Between groups | 493.602 | 2 | 683.52 | 5.940 | 0.000 |
| Within the group | 356.310 | 145 | 67.351 | |||
| total | 849.912 | 147 | ||||
Table 3: One-Way ANOVA Results
Table 4 shows the correlation test results of variables. According to Pearson correlation test, there is an absolute negative correlation between PDI, MDI and ultrasonic gray value at the level of 0.01 and the correlation coefficients are -0.830 and -0.917, respectively, indicating that the higher the score of PDI and MDI, the lower the ultrasonic gray value. It also indicated that the lower the PIVH and PWMD grades, the higher the PDI and MDI scores, the more mild the brain injury of premature infants and the better the brain development.
| PDI/MDI | Grey value | ||
|---|---|---|---|
| PDI | Pearson correlation | 1 | -0.830** |
| Significance (bilateral) | 0.000 | ||
| n | 148 | 148 | |
| Grey value | Pearson correlation | -0.830** | 1 |
| Significance (bilateral) | 0.000 | ||
| n | 148 | 148 | |
| MDI | Pearson correlation | 1 | -0.917** |
| Significance (bilateral) | 0.000 | ||
| n | 148 | 148 | |
| Grey value | Pearson correlation | -0.917** | 1 |
| Significance (bilateral) | 0.000 | ||
| n | 148 | 148 | |
Table 4: Correlation Test Results of Variables
WMD is easy to induce mental retardation or cerebral palsy, causing serious adverse effects on children’s health and population quality, and aggravating the burden on children’s families and society. Therefore, early detection and reasonable intervention are the key factors to improve the prognosis. Yang et al. [8] believed that WMD in premature infants was closely related to hypoxic ischemia, underdevelopment of brain and infection. However, early clinical symptoms are not obvious and non-specific. It’s impossible to tell based on the symptoms. When slight pathological changes occur in early stage, scientific intervention can effectively improve the prognosis and avoid disease progression. Imaging examination plays an important role in WMD screening of premature infants, among which cranial ultrasound has become the preferred method for screening the risk of brain development defects of premature infants due to its advantages such as reasonable price, convenient use and no radiation. Clinically, it is recommended that preterm infants with gestational age <30 w be examined by cranial ultrasound after birth and re-examined after correcting gestational age [9]. The brain injury of premature infants mainly included PIVH and PWMD. PIVH is mainly associated with the intracranial germinal matrix of preterm infants, which is located below the ependymal membrane and consists of primitive cells from the junction of the caudate nucleus head, lateral ventricle and thalamus. At 26 to 32 w of gestational age, the blood vessel wall was thinner and the germinal matrix structure was looser. When cerebral venous pressure increases, hypoxia and ischemia may cause vascular rupture and hemorrhage, and blood breaks through the ependymal membrane and enters the ventricle to form PIVH. PWMD is a functional injury caused by hypoxia and ischemia of white matter cells in brain tissue. Some domestic scholars have shown that the gray level of cerebral white matter ultrasound is positively correlated with the degree of injury, indicating that craniocerebral ultrasound is of great value in the diagnosis of brain injury in premature infants [10].
Growth retardation may occur after birth in infants with very or very low body weight due to early separation from the mother and various complications. However, early catch-up growth retardation can affect the development of nerve and intelligence [11]. Northam et al. [12] found that the white matter volume and Intelligence Quotient (IQ) of premature infants with PWMD were significantly lower than those of normal term infants, indicating that WMD has certain influence on the motor and intellectual development of premature infants. The results of this study showed that the motor and mental retardation rate of premature infants rated as grade IV by PIVH and PWMD was 100 %. The motor and mental retardation rates of premature infants with PWMD grade III were 50 % and 62.5 % respectively. The children with punctate, cluster and linear injuries in craniocerebral ultrasound examination showed a gradual decrease in motor and mental scores. These results indicate that the severity of preterm infants with brain injury can significantly affect the prognosis. In addition, neurons proliferate in the fetal brain at 3 to 4 mo of gestational age and neurons form after 5 mo. The white matter myelin sheath appears successively after birth, which is better than the arrangement and stratification of neurons, as well as the degree and development speed of synapse formation, and the gray value is also different [13]. Lan et al. [14] indicated that the ultrasonic grayscale value of the head can reflect the degree of injury in the detected area. The higher the degree of WMD, the higher the grayscale value will be, the greater the possibility of liquefaction, edema and necrosis, the worse the prognosis, and the greater the influence on the movement and intelligence of premature infants. Ultrasound gray value was detected in abnormal areas of white matter and the correlation between ultrasonic gray value and PDI and MDI was analyzed in abnormal children. The results showed that there was an absolute negative correlation between PDI, MDI and ultrasonic gray value. The smaller the gray value, the smaller the degree of WMD, the higher the PDI and MDI scores, better the long-term prognosis.
Chen et al. [15] followed up preterm infants with brain injury and found that neurodevelopmental treatment of preterm infants with abnormal postures and before immobilization of movement after brain injury could promote their normal movement and language development and reduce the probability of cerebral palsy and cognitive impairment. Liu et al. [16] also indicated that early effective intervention of brain injury can promote brain development and reduce long-term complications. Therefore, it is necessary to carry out regular follow-up and establish special management for premature infants. Combined with cranial ultrasound early detection, early diagnosis and early intervention, it can improve the long-term prognosis and reduce the probability of neurological disability in children, which is of great significance for the detection of premature brain injury, prediction of intelligence and motor nerve retardation in premature infants.
Acknowledgement:
This work was supported by the Nanjing Pukou Central Hospital.
Conflict of interests:
The authors declared no conflicts of interest.
References
- Rose J, Vassar R, Cahill-Rowley K, Guzman XS, Hintz SR, Stevenson DK, et al. Neonatal physiological correlates of near-term brain development on MRI and DTI in very-low-birth-weight preterm infants. Neuroimage Clin 2014;5:169-77.
[Crossref] [Google Scholar] [Pub Med]
- Niu Y, Fu J, Xue X. Magnetic resonance imaging of premature infants with punctate white matter damage and short-term neurodevelopmental outcome. Chin J Pediatr 2014;52(1):23-7.
- Bao X, Liu W. The application of neonatal behavioral neurometry and observation in the evaluation and early intervention of premature infants and infants' brain development. Chin J Pract Pediatr 2017;32(11):820-2.
- Yao Y, Hong J, Chen Q, Wu C. The effect of hypertension during pregnancy on neonatal brain damage and brain development. Chin J Med Ultrasound 2015;12(04):306-11.
- Hua Y, Chen Q. The value of MRI in evaluating the prognosis of children with hypoxic ischemic encephalopathy. J Int Pediatr 2017;44(9):602-6.
- Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: A study of infants with birth weights less than 1500 gm. J Pediatr 1978;92(4):529-34.
[Crossref] [Google Scholar] [Pub Med]
- He W, Shi C, Wang L, Liu G. Clinical and MRI analysis of brain injury and brain development in premature infants. J Jinan Univ 2015;36(1):62-7.
- Yang Q, Wang S. The pathogenesis of white matter damage in premature infants and new advances in early diagnosis methods. Med Rev 2014;20(2):228-31.
- Wang H, Liao H, Sun M. Analysis of the correlation between brain injury in premature infants and intrauterine infection during pregnancy. Tibetan Med 2017;38(3):12-5.
- Qin Z. Research progress on MRI evaluation of brain white matter damage and brain development in premature infants. Int J Pediatr 2019;5:327-30.
- Shi S. Observation on the effects of different degrees of brain injury in premature infants on the physical and neurodevelopment of infants. Qingdao Univ 2016.
- Northam GB, Liégeois F, Chong WK, Wyatt JS, Baldeweg T. Total brain white matter is a major determinant of IQ in adolescents born preterm. Ann Neurol 2011;69(4):702-11.
[Crossref] [Google Scholar] [Pub Med]
- Liu Z, Deng B, Jia X, Li B. A retrospective study of neuropsychological development in children with neonatal hypoxic-ischemic encephalopathy. Chin Matern Child Health Care 2015;30(23):3986-90.
- Lan F. The application value of craniocerebral ultrasound in premature infants with craniocerebral diseases. Imaging Res Med Appl 2017;1(13):162-3.
- Chen G, Zhang Y, Chen M, Wang X, Long Q, Kong Q, et al. Study on the early intervention model and clinical pathway of brain injury in premature infants. Chin J Contemp Pediatr 2014;16(1):35-9.
- Liu W, Bao X, Ma L, Wang D, Li X, Ren S, et al. Early intervention to reduce the incidence of cerebral palsy in very low birth weight infants. Chin J Child Health Care 2015;23(4):360-3.